Why Are Women at High Risk for Degenerative Arthritis?

Regen Health
2025-03-19

Osteoarthritis of the knee, also known as degenerative knee osteoarthritis (OA), is a common chronic joint disease primarily caused by the degeneration or damage of joint cartilage. This leads to a rough joint surface, loss of elasticity and smoothness, and may result in joint pain, stiffness, and limited mobility.
This condition is commonly seen in individuals over 50 years old, especially women and those who are overweight. In women, the decline in estrogen levels after menopause may affect bone health, increase the risk of osteoporosis, and make joint cartilage more prone to degeneration. Additionally, women generally have a wider pelvic structure and different knee joint angles compared to men, which may increase knee stress and contribute to the development of degenerative osteoarthritis.
Main Symptoms of Degenerative Osteoarthritis:
- Cartilage Degeneration: The joint cartilage gradually wears down, increasing friction between bones and affecting joint movement.
- Osteophyte Formation: To compensate for cartilage loss, bone spurs may form at the edges of the joint, worsening pain and discomfort.
- Joint Stiffness and Pain: Especially after activity or upon waking in the morning, joints often feel stiff and painful. Movement may temporarily relieve discomfort, but repeated use can exacerbate it.
- Limited Mobility: As the condition progresses, the range of motion of the joint may decrease, affecting daily activities.
Causes of Degenerative Knee Osteoarthritis:
Aging: As age increases, the cartilage in the knee gradually wears down.
Excess Weight: Carrying extra weight places additional stress on the knee joints, accelerating cartilage wear.
Overuse: Long-term excessive loading or intense exercise can cause knee joint damage.
Previous Injuries: Old knee injuries may accelerate the degenerative process.
Rheumatic and Autoimmune Diseases: Conditions such as rheumatoid arthritis can speed up knee joint degeneration.
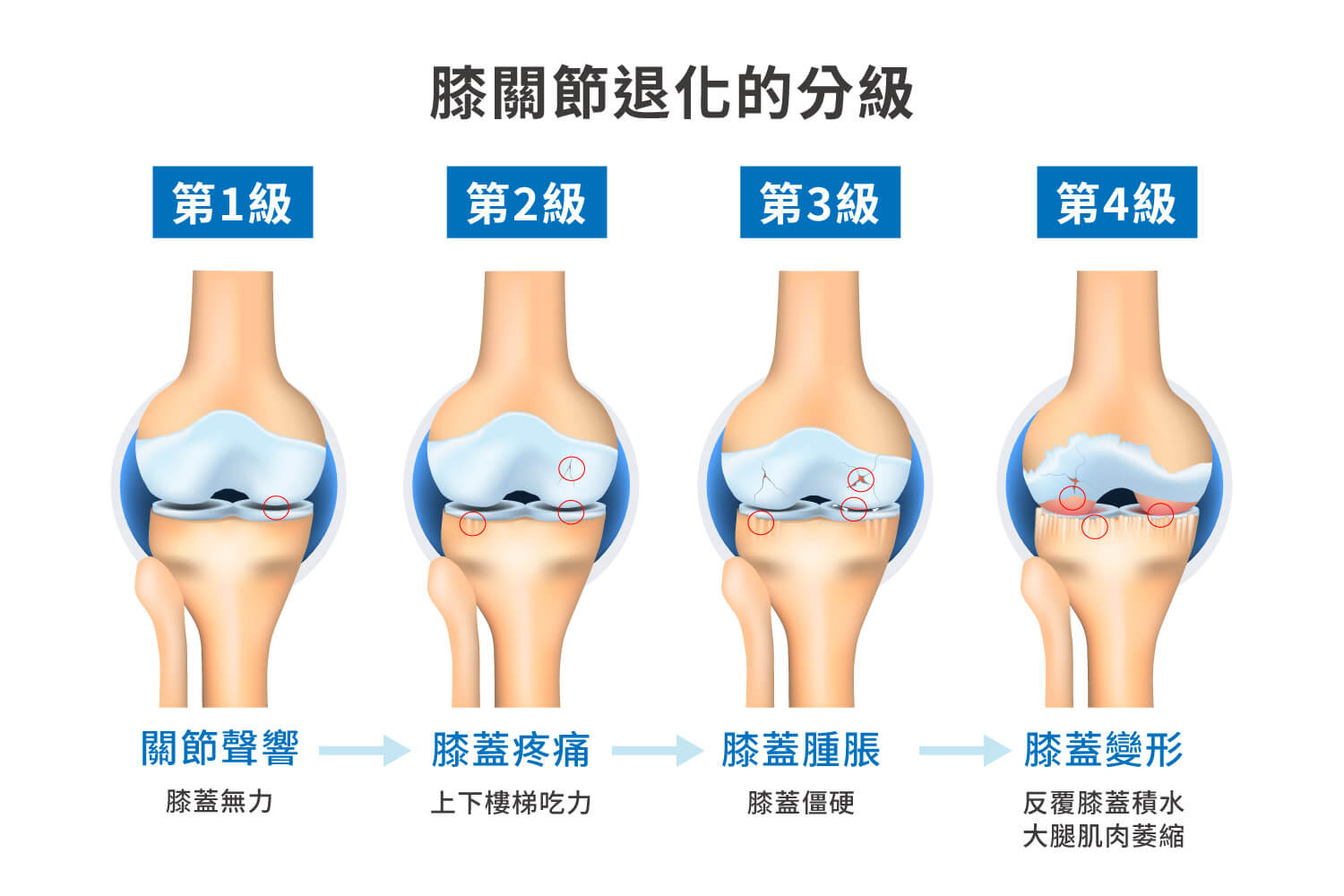
Grading of Knee Osteoarthritis:
Grade 1: Joint space slightly narrowed, possible small osteophytes.
Grade 2: Joint space narrowed, osteophytes clearly visible.
Grade 3: Joint space significantly narrowed, multiple osteophytes present.
Grade 4: Joint space lost, bones directly rub against each other causing deformation.
Common Treatment Methods:
- Injectable Therapy
Supplement the knee joint with cartilage nutrients, B12, and amino acids as needed. (Learn more) – hyperlink Comprehensive Bone & Joint IV Therapy - Ultrasound-Guided Joint Injection
Under real-time ultrasound guidance, autologous PRF high-concentration fibrin is injected to promote cartilage repair and regeneration, reducing inflammation and pain. (Learn more) – hyperlink Non-Surgical Joint Repair Therapy - Physical Therapy
High-intensity magnetic therapy: pain relief, anti-inflammation, improved circulation, and relaxation of tight muscles. - 1-on-1 Manual Therapy
Manual therapy: muscle strength training to increase joint stability and make knees more resilient. - Arthroscopic Surgery
Cartilage repair and regeneration procedure performed under sedation by an orthopedic surgeon, with better outcomes when combined with PRF therapy.
Four Postoperative Knee Exercises: Strengthen the Knee and Restore Mobility
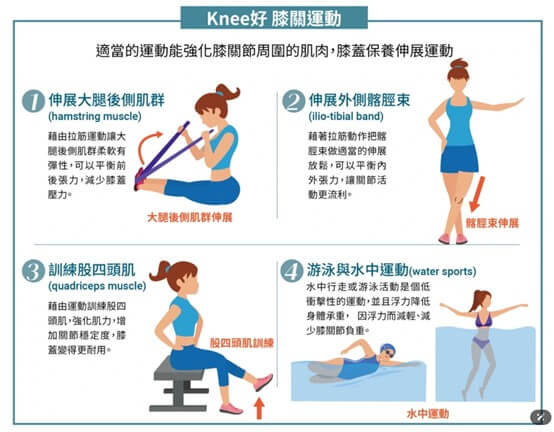
Appropriate postoperative exercises can effectively strengthen the muscles around the knee, help reduce joint stress, and promote recovery. The following four exercises are highly recommended for postoperative knee rehabilitation:
1. Hamstring Stretch – Stretching the muscles at the back of the thigh helps reduce anterior-posterior tension on the knee and alleviates knee pressure.
2. Iliotibial Band Stretch – Stretching the IT band improves medial-lateral tension of the knee, allowing smoother joint movement.
3. Quadriceps Strengthening – The quadriceps are crucial for supporting the knee joint; strengthening them increases knee stability and durability.
4. Water Walking or Swimming – Aquatic exercises are low-impact, and the buoyancy of water reduces knee load, making them ideal during postoperative recovery.
How to Prevent Degenerative Osteoarthritis:
The key to preventing knee osteoarthritis is maintaining knee health, reducing overuse and injury, and strengthening the surrounding muscles to support the joint. Here are some effective prevention strategies:
1. Maintain a Healthy Weight – Excess weight increases pressure on the knees, accelerating cartilage wear, especially when bearing heavy loads.
2. Proper Exercise and Muscle Strengthening – Choose low-impact exercises such as swimming, water walking, or cycling. These activities place less stress on the knees while strengthening muscles and maintaining joint health.
3. Avoid Overloading and Overuse – Prolonged standing, walking, or heavy lifting increases knee stress. Avoid high-intensity or overly strenuous activities that may overload the knee.
4. Regular Joint Checkups – For individuals with a history of knee problems or older adults, routine examinations help detect early signs of degeneration and allow timely interventions to slow progression. (Learn more) hyperlink Full Body Joint Checkup
Related Articles
Please enter a title here Hsu Fang-wei (Orthopedic Surgeon at Jianli Clinic) | Orthopedic Specialist License No. 002188 Please enter a title here What Is Piriformis Syndrome? A Common Nerve Compression Problem in People Who Sit for Long Periods Every time you walk into an office or a coffee shop, t
Please enter a title here Hsu Fang-wei (Orthopedic Surgeon at Jianli Clinic) | Orthopedic Specialist License No. 002188 Please enter a title here Lately, in my clinic, I often see middle-aged women rush in, looking panicked, pointing to the middle joint of their finger and asking, “Doctor, is my fin
For degenerative knee osteoarthritis, conventional treatments can only relieve pain, whereas PRP (platelet-rich plasma) and PRF (platelet-rich fibrin) work through six scientifically proven mechanisms—“promoting cartilage regeneration,” “modulating inflammation,” and “improving mitochondrial functio