Orthopedic Pain
Knee
Orthopedic pain
knee
Knee
Neck & Cervical Spine
Shoulder & Shoulder Joint
Elbow Joint
Wrist & Fingers
Lower Back & Lumbar Pain
Hip Joint
Knee
Ankle & Foot
Full Joint Checkup
Osteoarthritis (OA)

Table of Contents
What Is Osteoarthritis? Don’t Put Up With Joint Pain, Stiffness, and Cracking Any Longer: A Comprehensive Guide to Causes, Symptoms, Diagnosis, and Treatment
If you experience joint pain during physical activity, stiffness after sitting for long periods, difficulty climbing stairs, joint crepitus, or even find yourself reluctant to move due to pain, these symptoms aren’t necessarily just due to the weather or aging. Clinically, these symptoms are highly consistent with osteoarthritis (OA).
Osteoarthritis is not simply “inflammation,” but a continuous process of structural degeneration: cartilage wear → reduced cushioning → increased joint friction → inflammation and bone spur formation → pain and decreased function
What is Osteoarthritis?
Osteoarthritis is the most common chronic joint disease. The core pathology involves the wear and thinning of joint cartilage, leading to insufficient cushioning between bones and increased friction, which in turn results in:
- Pain and stiffness
- Joint swelling or fluid accumulation
- Reduced range of motion
- Joint instability and deformity
📍 Commonly affected areas:
knees, hips, fingers, and spine (weight-bearing or high-use joints)
Causes of Osteoarthritis (Clinically Proven)
- Advancing age: Decreased water content in cartilage and slower repair capacity
- Excess weight/chronic weight-bearing and overuse: For every 5 kg increase in body weight, the load on the knee joint can increase by approximately 15–20 kg
- Previous injuries and surgical history: Fractures, meniscus, or ligament injuries
- Abnormal joint alignment or structure: Uneven force distribution accelerates wear and tear
- Genetic and metabolic factors: Family history, sarcopenia, chronic low-grade inflammation
📊 A systematic review indicates that obese individuals have approximately twice the risk of developing knee osteoarthritis (OA) compared to those of normal weight.
(Felson et al., Annals of Internal Medicine, 1998)
Common Symptoms of Osteoarthritis: Which Type Do You Have?
- Early stage of joint
pain: pain on movement, relieved by
rest; late stage: persistent pain, night pain - Morning stiffness / stiffness after prolonged sitting (relieved by movement; a typical feature of OA)
- Swelling and effusion (synovial irritation, inflammatory response)
- Reduced range of motion (inability to bend or straighten the joint)
- Crepitus (clicking sounds)
- Deformity or instability, limping
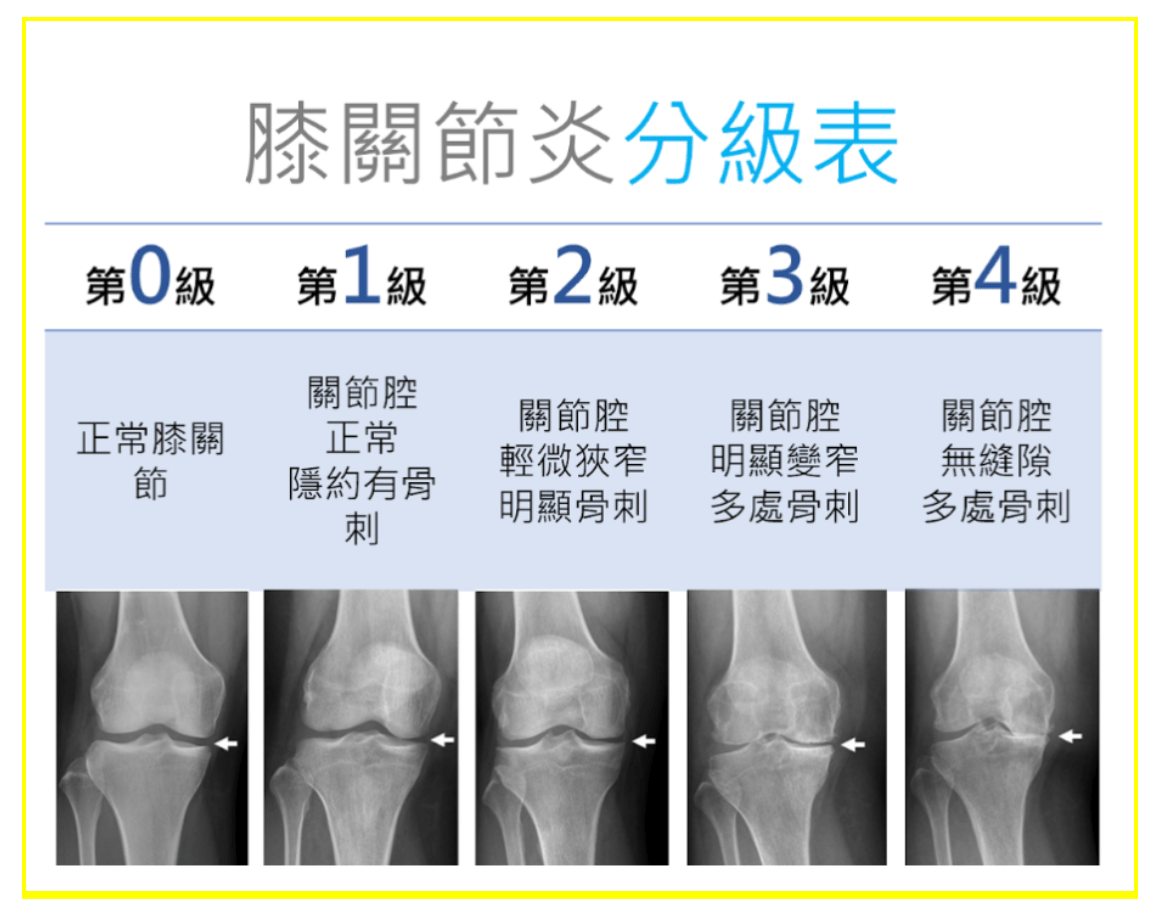
How is osteoarthritis diagnosed and clinically graded?
The physician will evaluate the patient based on symptoms, physical examination, and imaging studies:
- Physical examination: tenderness, range of motion, gait, muscle strength
- X-ray (first-line): Narrowing
of
the joint space, osteophytes,
subchondral sclerosis - Ultrasound: Effusion, synovial thickening, injection guidance
- MRI (when indicated): Changes in cartilage, meniscus, ligaments, and bone marrow
📚 International Guidelines: X-ray is the imaging modality of choice for OA; MRI is used when symptoms do not correlate with X-ray findings or for early assessment.
(ACR Appropriateness Criteria, 2022)
Populations Prone to Osteoarthritis
- Women aged 50 and older who have gone through menopause
- Obesity/metabolic syndrome
- Those who stand or walk for long periods, lift heavy objects, or engage in repetitive joint movements
- History of trauma or surgery
- Sarcopenia / Individuals with insufficient lower limb muscle strength
How to Prevent Osteoarthritis and Daily Care
- Weight Management: Losing 5–10% of body weight can significantly reduce pain
- Low-impact exercises: brisk walking, swimming, cycling, tai chi
- Strength Training: Quadriceps, Glutes, Core
- Posture and Movement Pattern Correction
- Early Assessment and Intervention
Common Treatments for Osteoarthritis
1️⃣ Conservative treatment (first-line)
- Medications: Acetaminophen, NSAIDs (risk assessment required)
- Physical therapy and exercise therapy
- Assistive devices: Knee braces, orthotics, canes
- Intra-articular injections:
Steroids (short-term, avoid frequent use); Hyaluronic
acid (lubrication and symptom relief)
2️⃣ Regenerative Therapy (PRP/PRF) Suitable
for recurrent pain, chronic inflammation, and patients seeking more aggressive intervention.
- Objective: To improve the inflammatory environment within the joint and promote the repair response
- Advantages: Autologous source, minimally invasive, short recovery period
- Clinical Evidence: Systematic reviews indicate that PRP is superior to hyaluronic acid alone in improving pain and function, particularly in mild to moderate OA.
(Dai et al., Arthroscopy, 2017; Cochrane Review, 2022)
3️⃣ Surgical Treatment (Rare)
- Minimally invasive arthroscopic surgery
- Total joint replacement (for advanced cases)
Frequently Asked Questions About Osteoarthritis
Is osteoarthritis just “normal as you get older”?
No. Aging increases the risk, but the progression can be significantly slowed through weight loss, strength training, and early treatment.
Why does it hurt more when the weather gets cold?
Cold stimulation can cause soft tissues to tighten, circulation to deteriorate, and pain to become more pronounced; keeping warm and warming up are very important.
How long is considered normal for morning stiffness?
Osteoarthritis commonly presents with stiffness upon waking or after prolonged sitting, which is relieved by activity. If morning stiffness persists for a long time and is accompanied by swelling and pain in multiple joints, it is necessary to differentiate it from other inflammatory joint diseases.
Does clicking or popping sound in the joints indicate degeneration?
Not necessarily. The sound could come from tendon slippage or uneven joint surfaces; further examination is needed if it is accompanied by pain, swelling, or locking.
Can people with osteoarthritis exercise?
Yes, and you should exercise. The key is low-impact and gradual progression, combined with strength training to protect your joints.
Can steroids be taken continuously?
Frequent injections are not recommended as they may affect the quality of cartilage and surrounding tissues; the timing and frequency should be assessed by a physician.
Are PRP/PRF really effective for osteoarthritis?
Clinically, it is often used to improve pain and function and reduce chronic inflammation recurrence; the effect is closely related to the degeneration grade, joint location, and combined muscle strength training, and needs to be evaluated before planning.
When should you seek medical attention for osteoarthritis?
If the pain lasts for more than 2–3 weeks, there is recurring swelling and fluid accumulation, a decrease in walking distance, nighttime awakening due to pain, or if it affects climbing stairs or daily activities, it is recommended to get checked as soon as possible.
Related Articles
CASE Testimonials Mr. Xie, the owner of Hongda International, has maintained a regular fitness routine for many years, yet he has been plagued by a five-year-old shoulder injury that prevented him from raising his arm smoothly and even caused him to wake up in pain when turning over in bed at night.
orthopedics Orthopedic pain Shoulder joint Text description, text description, text description, text description Table of Contents A Comprehensive Guide to Frozen Shoulder Treatment: Breaking the Vicious Cycle of Inflammation and Adhesions to Restore Shoulder Mobility Frozen shoulder (also known as