Orthopedic Pain
Hip Joint
Orthopedic pain
Hip joint
Hip Joint
Neck & Cervical Spine
Shoulder & Shoulder Joint
Elbow Joint
Wrist & Fingers
Lower Back & Lumbar Pain
Hip Joint
Knee
Ankle & Foot
Full Joint Checkup
Osteoarthritis of the hip
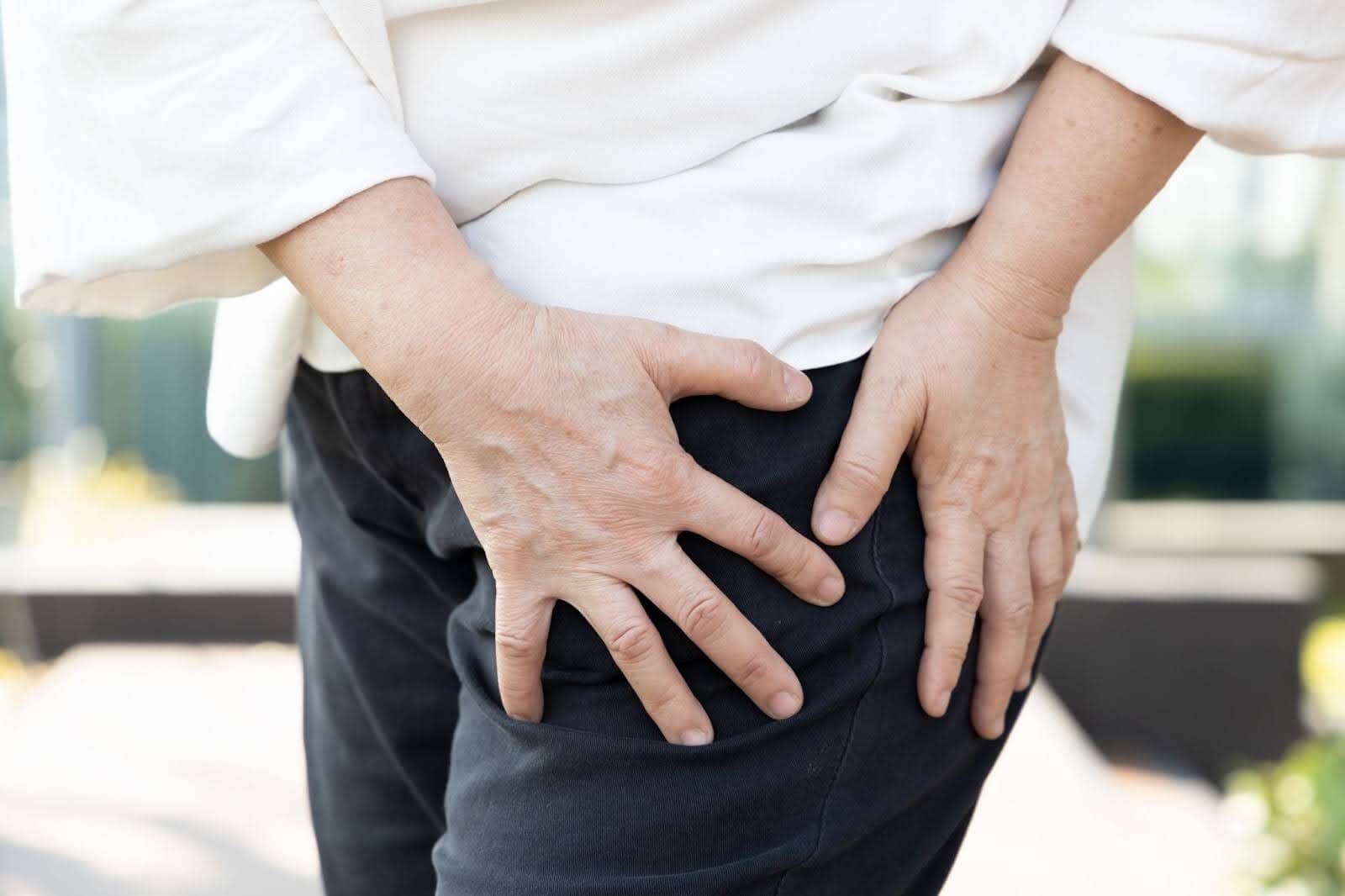
Table of Contents
What is degenerative hip arthritis? Groin pain, hip pain, knee pain, or a limp when walking? Learn the warning signs of hip degeneration first!
Do you experience pain in your groin, deep aching in your buttocks, or even pain in your knees?
Have you started limping when you walk, found it difficult to go up and down stairs, or even struggled with simple tasks like putting on socks or trimming your toenails?
These symptoms aren’t necessarily just due to aging or muscle fatigue; clinically, they are often early warning signs of hip osteoarthritis (Hip OA).
📊 Epidemiological data shows that approximately 10–12% of adults worldwide have symptomatic hip osteoarthritis, with a significant increase in the population aged 50 and older. It is one of the major factors affecting mobility and quality of life.
(Source: Global Burden of Disease Study, 2019)
What is osteoarthritis of the hip?
Osteoarthritis of the hip is a chronic degenerative joint disease caused by the gradual wear and thinning of the hip joint cartilage, leading to:
- increased friction between the joint surfaces
- Reduced cushioning and shock-absorbing capabilities
- Inflammation and bone spur formation
- Limited range of motion and pain
The hip joint, composed of the femoral head and the acetabulum, is one of the body’s largest weight-bearing joints. When
the cartilage degenerates, the bones rub directly against each other, which is the root cause of pain and stiffness.

Common Causes of Hip Osteoarthritis (Clinical Evidence)
- Age and natural wear and tear: Decreased hydration and elasticity of cartilage
- Long-term high stress or overuse: running, jumping, lifting heavy objects, prolonged standing
- Congenital hip dysplasia (DDH): Structural misalignment, premature degeneration
- History of trauma: altered joint alignment following fractures or dislocations
- Obesity and Genetic Factors: For every 5-point increase in BMI, the risk of hip degeneration rises significantly

Typical Symptoms of Osteoarthritis of the Hip: Why Does the Pain Radiate to Other Areas?
Pain associated with osteoarthritis of the hip often presents as referred pain:
- Groin pain (the most common)
- Deep buttock pain, lateral thigh pain
- Knee pain (often misdiagnosed as a knee joint problem)
- Stiffness after prolonged sitting or standing, which improves slightly with movement
- Limping and difficulty climbing or descending stairs
- Difficulty putting on socks or trimming toenails (restricted hip internal rotation)
📚 Clinical studies indicate that approximately 30–50% of patients with hip osteoarthritis present with knee pain as their primary complaint, leading to delayed diagnosis. (Khan et al., J Bone Joint Surg Br, 2004)
High-Risk Groups for Degenerative Hip Arthritis
- Ages 50 and older (women are at slightly higher risk, particularly after menopause)
- People who are overweight or experience frequent weight fluctuations
- Those who engage in high-impact sports or work that involves prolonged standing and heavy lifting
- Congenital hip dysplasia
- History of hip trauma or surgery
- Individuals who are sedentary, have weak hip muscles, or maintain poor posture
How is degenerative hip arthritis diagnosed? (Don’t just focus on where it hurts)
The doctor will conduct a comprehensive evaluation:
✔ Physical examination
- Range of motion of the hip joint
- Pain provocation tests
- Gait and pelvic stability
✔ Imaging studies
- X-ray (first-line): joint space, bone spurs, deformity
- MRI: Assessment of cartilage, labrum, bone marrow edema, and early-stage lesions
Treatment Options for Osteoarthritis of the Hip
1️⃣ Non-surgical treatment (primary approach for early- to mid-stage cases)
- Physical Therapy and Rehabilitation Exercises: To improve range of motion and muscle strength
- Medication: Short-term NSAIDs (as assessed by a physician)
- Intra-articular injections:
- Steroids: Short-term anti-inflammatory and pain relief
- Hyaluronic acid: Improves lubrication
- Regenerative/Proliferation Therapy:
- High-concentration glucose
- PRP (Platelet-Rich Plasma)
📊 A systematic review shows that PRP is superior to simple pain relief therapy in improving pain and function for mild to moderate hip osteoarthritis, but strict selection of indications is required. (Cochrane Review, 2022)
2️⃣ Surgical Treatment (Severe Functional Limitation)
- Arthroscopy (specific early-stage lesions)
- Osteotomy (for younger patients or those with structural abnormalities)
- Total hip replacement (advanced stages, success rate >90%)
Daily Care and Prevention of Osteoarthritis of the Hip (The Key to Slowing Progression)
- Weight Management (The Most Effective Approach)
- Get up and move around every 30–60 minutes
- Low-impact exercises: swimming, cycling, brisk walking
- Gluteus medius and core exercises
- When lifting heavy objects, bend your knees, not your waist
Frequently Asked Questions About Osteoarthritis of the Hip
Can hip joint degeneration be completely cured?
While cartilage wear and tear cannot be reversed, it can effectively reduce pain and slow down its progression.
Does hip joint degeneration always require surgery?
Most patients in the early to mid-stages can improve through non-surgical treatment.
Will exercise make things worse?
Incorrect sports activities; proper low-impact training combined with strength training can actually have a protective effect.
Is all hip pain a sign of degeneration?
No, it needs to be differentiated from bursitis, tendinitis, and lumbar nerve compression.
Will hip joint degeneration always get worse?
Not necessarily. The rate of deterioration is related to weight control, activity level, muscle strengthening exercises, and whether treatment is initiated early. With appropriate treatment and lifestyle adjustments, many patients can maintain stable condition for a long time without rapid deterioration.
Why does hip joint degeneration cause pain that extends to the knee?
This is a common type of “migrated pain.” The nerve pathways of the hip and knee joints partially overlap, so a lesion in the hip may manifest as pain in the thigh or knee. It is necessary to investigate the source to avoid misdiagnosis and treatment of only the knee.
Are PRP or regenerative therapy suitable for osteoarthritis of the hip?
Some patients with mild to moderate symptoms may benefit, but it is not suitable for everyone. Whether or not to proceed depends on imaging examinations, the degree of degeneration, and symptom assessment, with the doctor determining the most appropriate treatment strategy.
Do everyday postures really affect hip joint degeneration?
Yes. Prolonged sitting, crossing your legs, bending over to lift heavy objects, or weak hip muscles can all increase the burden on your joints. Improving posture and strengthening your glutes and core muscles can help reduce stress and slow down degeneration.
Related Articles
CASE Testimonials Mrs. Chen, 70, had suffered from osteoarthritis for many years. After several PRP treatments, she noticed a significant improvement: not only has her knee pain decreased dramatically, but she can now play with her grandchildren freely and has regained her mobility! Afraid of surgic
Regen Health SIS Super Magnetic Therapy Device: Medical-grade HIFEM technology—a powerful tool for chronic pain management! The SIS Super Inductive System (SIS) is an advanced non-invasive therapy that utilizes HIFEM (High-Intensity Focused Electromagnetic) technology. With an intensity of 2.5 Tesla