PRF

Regen Health
2026-02-15

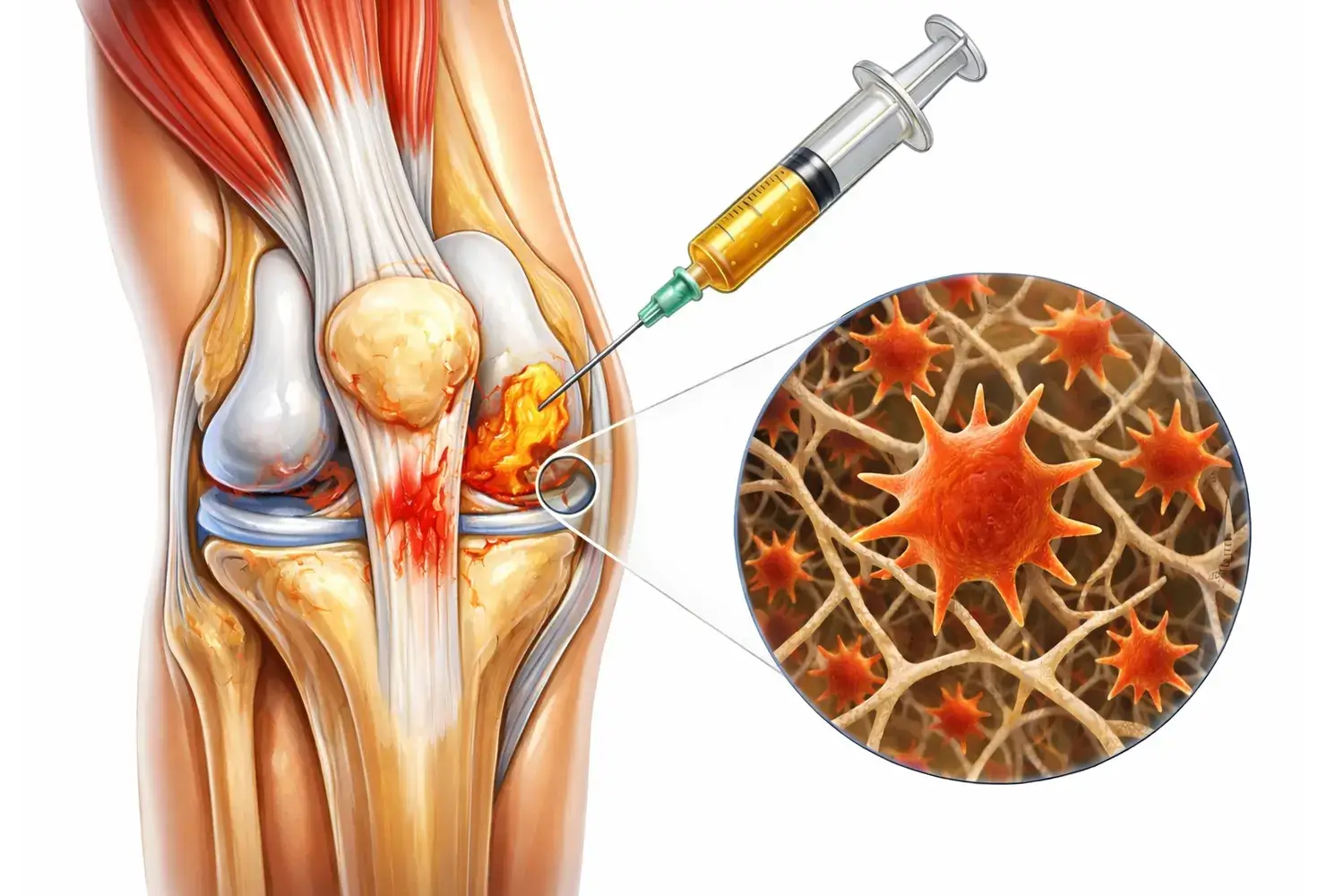
Advanced PRP Therapy | The Golden Treatment for Activating the "Self-Repair" Mechanism of Joints and Tendons
PRF is a highly safe, naturally derived regenerative medicine therapy that utilizes growth factors and fibrin structures from the patient’s own blood to help the body activate its tissue repair mechanisms. Compared to traditional PRP, PRF provides longer-lasting repair signals and a more stable environment for tissue regeneration, leading to its increasing application in the fields of orthopedics, sports medicine, and regenerative medicine.
Since PRF is derived entirely from the patient’s own blood and contains no drugs or artificial additives, it offers high safety and excellent biocompatibility. In recent years, it has been regarded as one of the most promising minimally invasive regenerative therapies in the fields of orthopedics, sports medicine, and regenerative medicine.
What is PRF?
PRF (Platelet-Rich Fibrin) can be considered an advanced form of PRP (Platelet-Rich Plasma).
Compared to traditional PRP, PRF retains the intact fibrin structure, allowing repair factors to remain more stably within the damaged tissue and exert their effects over a longer period.
PRF contains several key reparative components:
- High-concentration platelets: Initiate tissue repair responses
- Growth factors: Promote cell regeneration and angiogenesis
- Fibrin Matrix: Provides a three-dimensional scaffold for cell attachment
- Autologous exosomes: Transmit cellular repair signals
- Cell Activators: Promote the initiation of self-repair in damaged tissues
These components help achieve anti-inflammatory effects, reduce pain, and promote tissue regeneration, making PRF an increasingly important treatment option in regenerative medicine.
Features and Benefits of PRF Therapy
PRF has garnered attention in the field of regenerative medicine primarily due to the following advantages:
1. Autologous source and high safety: It avoids rejection or allergic reactions caused by foreign substances.
2. Longer retention time in gel form: Repair factors can maintain a higher concentration at the affected site.
3. Sustained-release of growth factors: Repair signals can continue to act for several weeks.
4. Reduces inflammation and alleviates chronic pain: Suitable for various joint and tendon conditions.
5. Three-dimensional structure promotes tissue regeneration: Supports the repair of cartilage, tendons, and ligaments.
6. Wide range of applications: Concentration and formulation can be adjusted based on the treatment site.
Who is PRF therapy suitable for?
- Patients who do not wish to undergo surgery or are unable to do so: Patients who hope to delay joint replacement through conservative treatment.
- Athletes with sports injuries: Athletes with torn tendons or ligaments who require precise repair to return to competition.
- Those who have had ineffective blind injections: Patients who have previously received hyaluronic acid or PRP injections with poor results—likely due to imprecise placement—may benefit from ultrasound-guided PRF.
- Those allergic to anticoagulants or who prefer natural treatments: PRF is 100% autologous and contains no chemical additives.
Standard Procedure for PRF Minimally Invasive Injections
| Comparison Criteria | PRP (Platelet-Rich Plasma) | PRF (Platelet-Rich Fibrin) |
|---|---|---|
| Addition of Anticoagulant | Yes (required to prevent blood clotting) | None (100% natural, no chemical additives) |
| Physical Form | Liquid (highly fluid) | Three-dimensional mesh gel (features a physical scaffold structure) |
| Growth factor release rate | Rapid release (completely released within a few days after injection) | Sustained-release (stable release in the body for up to 7–14 days) |
| Cell growth scaffold | No physical scaffold | Present (natural fibrin mesh that attracts stem cells to adhere and grow) |
| Clinical Indications | Mild to moderate osteoarthritis, extensive superficial inflammation, general tendinitis, muscle strains. | Deep ligament/tendon tears, cartilage defects, chronic pain and inflammation, tissue reconstruction. |
Clinical Applications of PRF Therapy
PRF is currently used in a number of medical fields, including:
1. Orthopedics and Sports Medicine
PRF can help reduce pain, alleviate inflammation, and enhance tissue repair capabilities. Common indications include:
- Osteoarthritis (knee OA)
- Meniscal or cartilage wear
- Frozen shoulder, rotator cuff injuries
- Tennis elbow, golfer’s elbow
- Plantar fasciitis
- Mild ligament tears (MCL, ATFL)
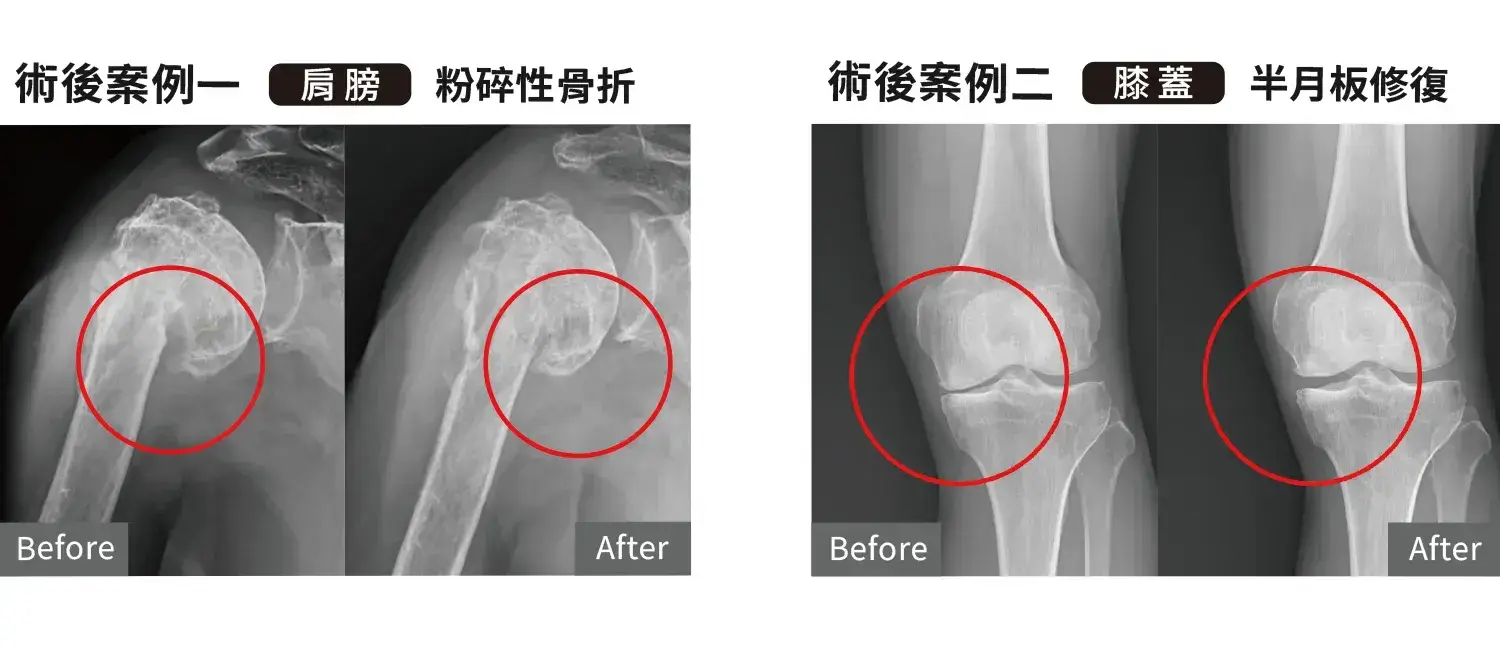
2. Post-surgical recovery
PRF is also frequently used in conjunction with surgery to enhance tissue repair quality. For example:
- Delayed fracture healing
- Post-arthroscopic surgery recovery
- Meniscus or cartilage repair
3. Regenerative Medicine and Aesthetic Medicine
As an autologous therapy, it offers a high level of safety. Common applications include:
- Improvement of fine lines and skin laxity
- Improving dark circles
- Repair of acne scars
- Facial tissue repair
4. Dental Regenerative Therapy
PRF is also widely used in dentistry to promote the healing of bone and periodontal tissues. For example:
- Dental implant surgery
- Bone grafting
- Periodontal Tissue Repair
Note: PRF is a form of regenerative medicine; its actual efficacy and indications must be determined by a qualified dentist following a professional evaluation.
PRF Therapy FAQ
Q1: Does PRF treatment hurt?
The PRF treatment process typically involves only a brief sensation of soreness or pressure. Most procedures are performed under local anesthesia or ultrasound guidance, so any discomfort is usually within an acceptable range. After treatment, you may experience mild tightness or soreness in the treated area, which usually subsides gradually within 1–3 days.
Q2: Does PRF cause an immune rejection reaction?
PRF is derived 100% from the patient’s own blood and contains no foreign drugs or artificial additives, so it rarely causes immune rejection or allergic reactions. Due to its high biocompatibility, it is considered one of the safer regenerative medical therapies.
Q3: How long does it take to see results from PRF?
PRF works by gradually activating the body’s natural tissue repair mechanisms to improve symptoms, so results are typically not immediate.
The actual recovery rate varies depending on the severity of the injury, the treatment site, and individual constitution. The general recovery timeline is as follows:
- 2–6 weeks: Pain relief begins to be felt
- 1–3 months: Tissue repair becomes gradually apparent
- 3–6 months: Tissue reconstruction and stabilization phase
Q4: How many PRF treatment sessions are required?
Most patients are recommended to undergo 1–3 sessions; the actual number will be determined by the physician based on individual circumstances, such as:
- Type of injured tissue (tendons, ligaments, or cartilage)
- Duration of the condition
- Degree of tissue degeneration or damage
- Individual healing capacity
Q5: Can PRF replace surgery?
PRF is more suitable for mild to moderate tissue damage or early-stage degenerative conditions, such as:
- Early-stage osteoarthritis
- Chronic tendinitis
- Mild ligament tears
- Plantar fasciitis
In cases of severe joint degeneration, complete ligament rupture, or structural damage, surgical treatment may still be necessary. PRF is also commonly used post-surgery to accelerate recovery and improve healing outcomes.
Q6: What is the difference between PRF and PRP?
PRF is often considered an advanced version of PRP (platelet-rich plasma), so PRF provides a more stable tissue repair environment and longer-lasting repair signals.
The main differences between the two lie in their structure and mechanism of action:
- PRP: A liquid platelet concentrate with a faster release of growth factors
- PRF: Features a fibrin mesh structure, forming a gel-like healing environment
Q7: Is PRF treatment covered by national health insurance?
Currently, PRF and ultrasound-guided injections are generally considered out-of-pocket services. Although the cost is higher, due to their high precision and safety, and the fact that they use the patient’s own blood with no risk of rejection, they represent an extremely cost-effective option for regenerative medicine.
Q8: Who is not suitable for PRF treatment?
Patients with abnormal platelet function, severe anemia, blood-borne infectious diseases, acute infections at the injection site, or those currently taking anticoagulant medications must be evaluated by a physician.
Frequently Asked Questions
What is PRP? How is it different from a regular painkiller injection?
PRP uses autologous blood to concentrate growth factors to initiate tissue repair and regeneration; painkillers mainly suppress pain temporarily, while PRP is a “root cause” treatment.
Who is PRP suitable for?
Suitable for patients with osteoarthritis, chronic tendon/ligament injuries, sports injuries, and those who wish to delay surgery or slow down joint aging.
How many PRP treatments are needed? How often should they be administered?
It is generally recommended to inject once every 3 to 4 weeks, and a complete course of treatment requires about 3 to 4 injections, depending on the severity of the condition as assessed by a physician.
What is the difference between PRP and hyaluronic acid (HA)?
Hyaluronic acid primarily provides joint “lubrication” and “shock absorption,” with effects lasting approximately 3-6 months; PRP, on the other hand, initiates “regeneration and repair,” resulting in longer-lasting effects (approximately 6-12 months or more).
How long does it take for PRP injections to take effect? How long do the effects last?
PRP provides non-immediate pain relief, with most patients experiencing improvement within one month, and the most significant repair effect after two to three months; some studies show that the effect can last for more than a year.
Will it hurt after the injection? How can I relieve the side effects?
There may be temporary soreness during the injection. If you feel unwell 3-7 days after the procedure, you can apply warm compresses (or ice packs) multiple times to relieve the soreness and pain, and take Acetaminophen. However, remember not to use anti-inflammatory drugs.
Who is not suitable for PRP? (Contraindications)
Direct injection is not recommended for individuals with platelet dysfunction, sepsis, acute/chronic infectious diseases, active infection of the affected area, immune system diseases, malignant tumors, pregnant women, or those taking anticoagulants long-term.
How much does PRP cost? Is there insurance coverage?
Currently, PRP is a fully out-of-pocket procedure and is not covered by health insurance. The cost per procedure ranges from approximately NT$15,000 to NT$20,000. If the injury is due to an accident or qualifies for outpatient surgery/hospitalization, reimbursement-based insurance policies often cover the costs. It is recommended to consult an insurance agent to confirm the policy terms before undergoing the procedure.
Frequently Asked Questions About PRP Treatment
Q1: What is PRP? How is it different from a standard painkiller injection?
PRP uses growth factors concentrated from the patient’s own blood to stimulate tissue repair and regeneration; painkiller injections primarily provide temporary pain relief, whereas PRP is a “root-cause” treatment.
Q2: Who is PRP suitable for
? It is suitable for patients with osteoarthritis, chronic tendon/ligament injuries, and sports injuries, as well as those who wish to delay surgery or slow down joint aging.
Q3: How many PRP sessions are needed? How often should they be administered? It is generally
recommended to have injections every 3 to 4 weeks. A full course typically requires 3 to 4 sessions, though the specific number will be determined by the physician based on the severity of the condition.
Q4: What is the difference between PRP and hyaluronic acid (HA)? Hyaluronic
acid primarily provides joint “lubrication” and “shock absorption,” with effects lasting approximately 3–6 months; PRP, on the other hand, triggers “regenerative repair,” offering longer-lasting results (approximately 6–12 months or more).
Q5: How long does it take for PRP injections to take effect? How long do the results last?
PRP does not provide immediate pain relief; most patients notice improvement within 1 month, with the most significant repair effects appearing after 2 to 3 months; some studies indicate that the effects can last for over a year.
Q6: Will it hurt after the injection? How can side effects be alleviated?
You may experience temporary soreness or swelling during the injection. If discomfort persists for 3–7 days post-procedure, apply warm compresses (or ice packs to relieve swelling and pain) as needed and take acetaminophen (Paracetamol), but remember never to use anti-inflammatory medications.
Q7: Who is not suitable for PRP? (Contraindications) PRP is not recommended for
individuals with platelet dysfunction, sepsis, acute or chronic infectious diseases, active infections at the treatment site, immune system disorders, malignant tumors, pregnant women, or those taking anticoagulants long-term.
Q8: How much does PRP cost? Is it covered by insurance? Currently
, PRP is a fully out-of-pocket procedure and is not covered by national health insurance. The cost per session ranges from approximately NT$15,000 to NT$20,000. If the injury is caused by an accident or meets the criteria for outpatient surgery or procedures, many indemnity-type insurance policies may provide coverage. It is recommended to consult an insurance agent to confirm policy terms before undergoing the procedure.
Related Articles
CASE Testimonials What Can Be Done About Recurrent Knee Pain Due to Degenerative Conditions? For many middle-aged and older adults, degenerative knee conditions often lead to a sharp decline in quality of life. Mr. Wu, an avid cyclist, has been suffering from recurring knee pain for over three month