PRP

Regen Health
2026-02-20

Say Goodbye to Joint Degeneration and Chronic Pain: A Guide to PRP Regenerative Therapy Injections, Cost Estimates, and Non-Surgical Treatment
PRP (Platelet-Rich Plasma) therapy is a clinically proven, non-surgical regenerative medicine technique. By drawing approximately 10–15 cc of the patient’s own blood and processing it through medical-grade centrifugation equipment, platelets and growth factors are purified to a concentration 3 to 5 times higher than that found in normal blood.This solution is then precisely injected into the affected joint or tendon, directly activating the body’s natural tissue repair mechanisms.
Are you suffering from these pains? Common Indications for PRP
- Lower Limb and Weight-Bearing Joints: Osteoarthritis of the knee (most effective in stages 1–3), anterior cruciate ligament (ACL) tears, meniscus injuries, and chronic plantar fasciitis.
- Upper Limb and Mobile Joints: Frozen shoulder (adhesive capsulitis), rotator cuff tears, tennis elbow, golfer’s elbow.
- Spinal and Perineural Conditions: Chronic lower back pain, lumbar facet joint syndrome.
Orthopedic Experts Explain: The 3 Key Factors That Determine the Efficacy of PRP Therapy
At Jianli Clinic, we believe that “giving an injection” is merely a physical act; the true medical value lies in precision and safety:
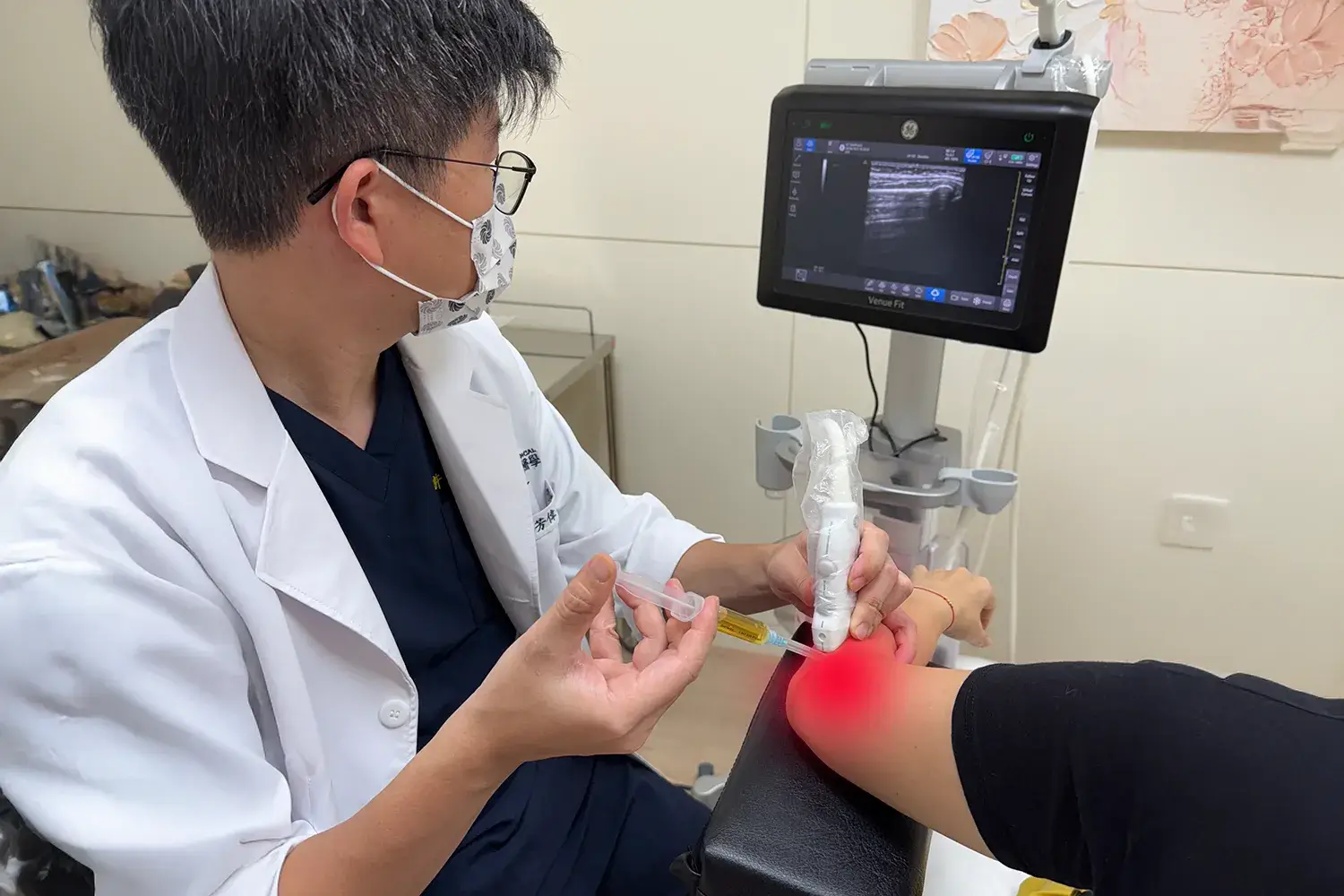
- High-Resolution Musculoskeletal Ultrasound-Guided Injection: Traditional “blind injections,” which rely on the physician’s tactile sense, can easily result in precious growth factors being injected into surrounding healthy tissue. Our clinic exclusively uses high-frequency ultrasound imaging to precisely avoid nerves and blood vessels, delivering PRP with pinpoint accuracy to tiny cartilage defects or ligament tear sites.
2. Customized Centrifugation Parameters and Concentration Control: Not all PRP is created equal. We dynamically adjust the centrifuge’s rotation speed (RPM) and duration based on the patient’s age, lesion depth, and severity to ensure the extraction of platelets with optimal activity (including adjustment of the white blood cell ratio).
3. Aseptic Technique: Blood collection and preparation are performed in a high-standard sterile environment to eliminate the risk of joint cavity infection.
Standard Procedure for PRP Minimally Invasive Treatment
| Steps | Item | Description |
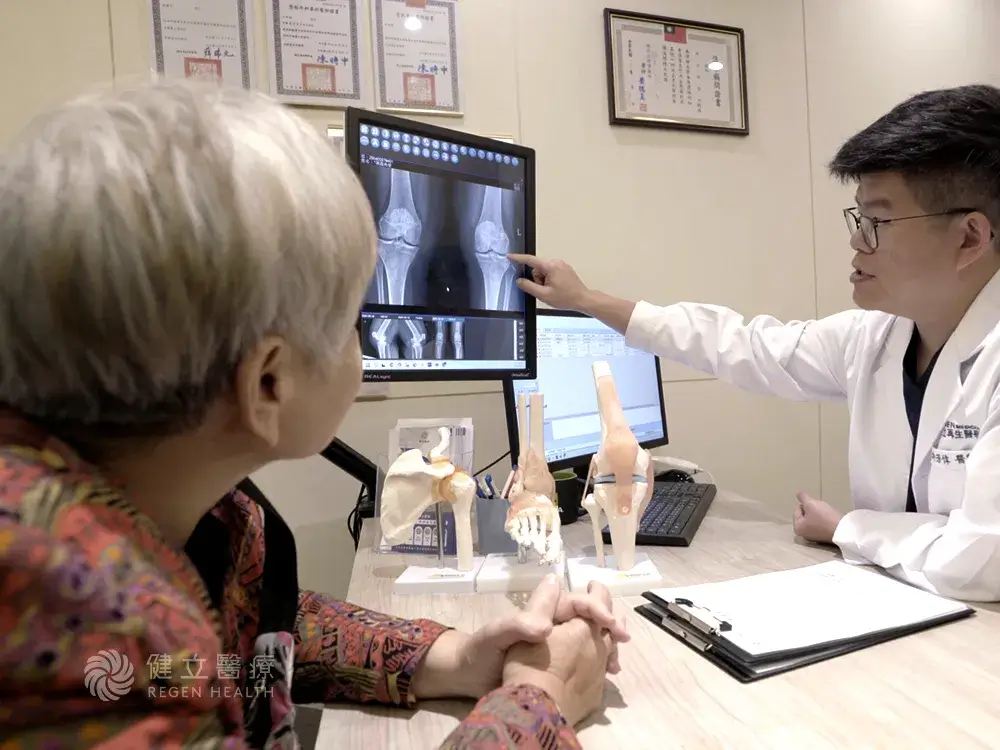
| STEP 1 | Professional Evaluation | The physician will perform a physical examination and use ultrasound to locate the affected area to determine if the patient is a suitable candidate for PRP. |
| STEP 2 | Sterile Blood Draw | A professional nurse draws the patient’s own blood (approximately 10–15 cc) without adding any anticoagulants. |
| STEP 3 | Customized Centrifugation | After blood collection, a medical-grade centrifuge operating at a specific speed is used to extract a "three-dimensional mesh gel-like" PRF scaffold rich in high concentrations of platelets, white blood cells, and growth factors. |
| STEP 4 | Guided Injection | After local disinfection, the physician performs a minimally invasive injection under precise ultrasound guidance. |
| STEP 5 | Post-Procedure Instructions | Patients may return home after a 15-minute observation period if no discomfort is reported. A nurse will provide a comprehensive post-procedure care guide. |
What You Need to Know About PRP Treatments: Side Effects and Post-Treatment Care Guidelines
Normal healing response: Within 3–7 days after the injection, you may experience soreness, tightness, pain, or slight swelling in the treated area. This indicates that the tissue is reorganizing; applying a warm compress is recommended for relief.
Absolute Contraindications: Strictly avoid taking anti-inflammatory drugs (NSAIDs) one week before and after the procedure, as they inhibit platelet-mediated healing! If experiencing severe pain, only take acetaminophen.
Nutritional Supplements: It is strongly recommended to increase your intake of vitamin C (approximately 1,000 mg daily), high-quality protein, and collagen to provide your body with ample “building materials” for healing.
Frequently Asked Questions (FAQ) About PRP Regenerative Therapy
Q1: How many PRP treatments are needed? How often should they be administered?
To achieve optimal tissue regeneration, it is generally recommended to receive a treatment every 3 to 4 weeks, with a full course consisting of approximately 3 to 4 sessions. The exact number of sessions will be determined by the physician based on the severity of the injury.
Q2: When will the pain subside after a PRP treatment?
PRP is not an instant pain reliever. Most patients will experience pain relief within one month, and tissue repair reaches its peak after 2 to 3 months, when the effects are most pronounced.
Q3: Who should not receive PRP treatment?
PRP is not recommended for individuals with platelet dysfunction, sepsis, acute or chronic infectious diseases, active infection or inflammation at the treatment site, immune system disorders, malignant tumors, or those taking anticoagulants long-term.
Q4: How much does PRP cost?
Is it covered by insurance? Currently, PRP is a self-pay procedure not covered by national health insurance. The cost per session ranges from approximately NT$15,000 to NT$20,000, depending on the equipment used. If the injury resulted from an “accident” or meets the “outpatient surgery” clause in your policy, indemnity-type insurance plans often provide coverage. We recommend consulting your insurance advisor before undergoing the procedure.
Frequently Asked Questions
What is PRP? How is it different from a regular painkiller injection?
PRP uses autologous blood to concentrate growth factors to initiate tissue repair and regeneration; painkillers mainly suppress pain temporarily, while PRP is a “root cause” treatment.
Who is PRP suitable for?
Suitable for patients with osteoarthritis, chronic tendon/ligament injuries, sports injuries, and those who wish to delay surgery or slow down joint aging.
How many PRP treatments are needed? How often should they be administered?
It is generally recommended to inject once every 3 to 4 weeks, and a complete course of treatment requires about 3 to 4 injections, depending on the severity of the condition as assessed by a physician.
What is the difference between PRP and hyaluronic acid (HA)?
Hyaluronic acid primarily provides joint “lubrication” and “shock absorption,” with effects lasting approximately 3-6 months; PRP, on the other hand, initiates “regeneration and repair,” resulting in longer-lasting effects (approximately 6-12 months or more).
How long does it take for PRP injections to take effect? How long do the effects last?
PRP provides non-immediate pain relief, with most patients experiencing improvement within one month, and the most significant repair effect after two to three months; some studies show that the effect can last for more than a year.
Will it hurt after the injection? How can I relieve the side effects?
There may be temporary soreness during the injection. If you feel unwell 3-7 days after the procedure, you can apply warm compresses (or ice packs) multiple times to relieve the soreness and pain, and take Acetaminophen. However, remember not to use anti-inflammatory drugs.
Who is not suitable for PRP? (Contraindications)
Direct injection is not recommended for individuals with platelet dysfunction, sepsis, acute/chronic infectious diseases, active infection of the affected area, immune system diseases, malignant tumors, pregnant women, or those taking anticoagulants long-term.
How much does PRP cost? Is there insurance coverage?
Currently, PRP is a fully out-of-pocket procedure and is not covered by health insurance. The cost per procedure ranges from approximately NT$15,000 to NT$20,000. If the injury is due to an accident or qualifies for outpatient surgery/hospitalization, reimbursement-based insurance policies often cover the costs. It is recommended to consult an insurance agent to confirm the policy terms before undergoing the procedure.
Frequently Asked Questions About PRP Treatment
Q1: What is PRP? How is it different from a standard painkiller injection?
PRP uses growth factors concentrated from the patient’s own blood to stimulate tissue repair and regeneration; painkiller injections primarily provide temporary pain relief, whereas PRP is a “root-cause” treatment.
Q2: Who is PRP suitable for
? It is suitable for patients with osteoarthritis, chronic tendon/ligament injuries, and sports injuries, as well as those who wish to delay surgery or slow down joint aging.
Q3: How many PRP sessions are needed? How often should they be administered? It is generally
recommended to have injections every 3 to 4 weeks. A full course typically requires 3 to 4 sessions, though the specific number will be determined by the physician based on the severity of the condition.
Q4: What is the difference between PRP and hyaluronic acid (HA)? Hyaluronic
acid primarily provides joint “lubrication” and “shock absorption,” with effects lasting approximately 3–6 months; PRP, on the other hand, triggers “regenerative repair,” offering longer-lasting results (approximately 6–12 months or more).
Q5: How long does it take for PRP injections to take effect? How long do the results last?
PRP does not provide immediate pain relief; most patients notice improvement within 1 month, with the most significant repair effects appearing after 2 to 3 months; some studies indicate that the effects can last for over a year.
Q6: Will it hurt after the injection? How can side effects be alleviated?
You may experience temporary soreness or swelling during the injection. If discomfort persists for 3–7 days post-procedure, apply warm compresses (or ice packs to relieve swelling and pain) as needed and take acetaminophen (Paracetamol), but remember never to use anti-inflammatory medications.
Q7: Who is not suitable for PRP? (Contraindications) PRP is not recommended for
individuals with platelet dysfunction, sepsis, acute or chronic infectious diseases, active infections at the treatment site, immune system disorders, malignant tumors, pregnant women, or those taking anticoagulants long-term.
Q8: How much does PRP cost? Is it covered by insurance? Currently
, PRP is a fully out-of-pocket procedure and is not covered by national health insurance. The cost per session ranges from approximately NT$15,000 to NT$20,000. If the injury is caused by an accident or meets the criteria for outpatient surgery or procedures, many indemnity-type insurance policies may provide coverage. It is recommended to consult an insurance agent to confirm policy terms before undergoing the procedure.
Related Articles
CASE Testimonials Mrs. Chen, 70, had suffered from osteoarthritis for many years. After several PRP treatments, she noticed a significant improvement: not only has her knee pain decreased dramatically, but she can now play with her grandchildren freely and has regained her mobility! Afraid of surgic
orthopedics Orthopedic pain Shoulder joint Text description, text description, text description, text description Table of Contents A Comprehensive Guide to Frozen Shoulder Treatment: Breaking the Vicious Cycle of Inflammation and Adhesions to Restore Shoulder Mobility Frozen shoulder (also known as