Pain and Anesthesia
Nerve Block Injection
Pain and Anesthesia
Nerve Block Injection
Nerve Block Injection
Various Anesthesia
Nerve Block Injection
Chronic Pain Management
Epidural Spinal Injection
Table of Contents
What is an epidural injection (ESI)?
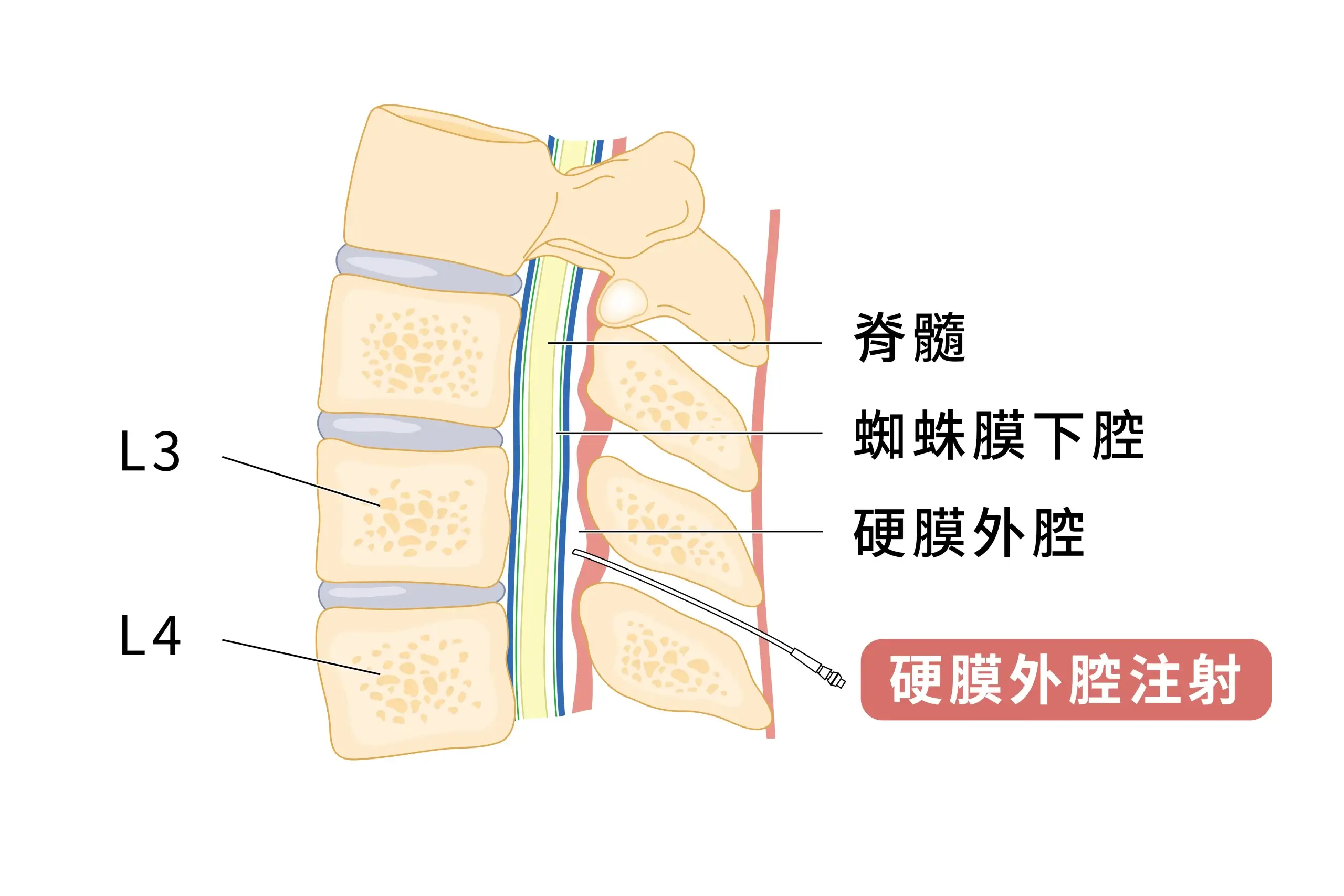
Epidural injections deliver a combination of "local anesthetics and steroids" directly to the inflamed nerves, reducing inflammation and swelling while blocking pain signals. This treatment is suitable for radiating pain associated with conditions such as herniated discs, sciatica, and spinal stenosis. When guided by X-ray or ultrasound, the procedure is even more precise and safe.
The epidural space lies between the spinal cord and the bony structures of the spine. It contains fatty tissue, blood vessels, lymphatic vessels, and nerve roots. An epidural steroid injection (ESI) involves injecting a mixture of local anesthetic and steroids into the epidural space, where it acts directly on the area surrounding the inflamed nerve. The primary objectives are:
- Reduce nerve swelling and inflammation
- To reduce the transmission of pain signals
- To alleviate symptoms such as sciatica and herniated discs
The procedure is typically performed in the lumbar or thoracic spine and is guided by X-ray or ultrasound to enhance safety and precision. In most cases, ESI is used as a short-term adjunct for pain relief and can serve as a bridging option between conservative treatment and surgery.
How does epidural injection (ESI) differ from other treatments?
- Conventional pain relief injections: Intramuscular injections or intravenous infusions enter the systemic circulation, resulting in shorter-lasting effects and a lack of local specificity; ESI targets the site of the problem directly and provides longer-lasting relief.
- Surgery: ESI does not alter anatomical structures and is intended for symptom management; however, if there is progressive nerve damage or cauda equina syndrome, surgery remains the preferred option.
- Frequency limit: To avoid steroid side effects (osteoporosis, immunosuppression, worsening blood sugar levels), do not exceed 3–4 times per year, and combine with physical therapy and core training to prolong the pain-free period.
| Treatment | Standard pain relief injections/infusions | Spinal Epidural Injection (ESI) |
|---|---|---|
| Site of Action | Systemic circulation; no specific site | Directly injected into the epidural space of the spine, acting on the area surrounding the inflamed nerve |
| Duration of Effect | Short-term (several hours to several days) | Weeks to months, depending on individual constitution and condition |
| Purpose | Short-term pain relief | Anti-inflammatory, reduces nerve swelling, alleviates pain, and facilitates rehabilitation |
| Invasiveness | Low | Moderate (requires image guidance and precise injection) |
| Recovery time | Almost immediate recovery | Can go home the same day; return to daily activities within 1–3 days |
| Suitable for | Acute pain, short-term relief | For those for whom conservative treatment has been ineffective and who are not suitable candidates for surgery |
Who is a good candidate for epidural injections (ESI)?
- Herniated disc, spinal stenosis
- Sciatica, tingling or numbness in the lower limbs
- Nerve root disorders and compression-related issues caused by facet joint arthritis, spinal stenosis, etc.
- Degenerative disc disease, chronic low back pain (following professional evaluation)
Who is not recommended to participate or needs to postpone?
- Active infection, fever, or skin infection at the injection site
- Poorly controlled diabetes or hypertension
- Current use of anticoagulant or antiplatelet medications without a completed risk assessment
- Pregnancy requires individualized assessment
- Moderate to severe allergy to local anesthetics or corticosteroids
- Severe coagulation disorders or thrombocytopenia
- Recent surgery at the same site or symptoms requiring immediate surgery (e.g., progressive neurological deficits, cauda equina syndrome)
Important Note: If you are taking anticoagulants or antiplatelet medications, please be sure to inform your physician. Follow your physician’s instructions to temporarily discontinue or adjust your medication before the injection to reduce the risk of bleeding or complications. To
learn more about epidural spinal injection (ESI) treatment options, please visit the Treatment Procedures page (hyperlink).
Frequently Asked Questions About Epidural Injections
How is epidural injection (ESI) performed?
Under ultrasound or X-ray guidance, the doctor will precisely locate the inflamed nerve and inject the medication into the epidural space of the spine.
The medication typically contains:
Local anesthetic: provides immediate nerve paralysis and temporary pain relief (lasting approximately half a day to a day).
Steroids: require 3–5 days to exert their anti-inflammatory effects and can prolong the pain relief, often lasting for weeks to months.
What is the difference between ESI and regular pain relief injections?
Conventional pain-relieving injections: These typically use morphine or anti-inflammatory analgesics, administered via intramuscular injection or intravenous drip into the systemic circulation. Their effects last only a few hours and lack specificity.
ESI injections: These inject the medication directly into the nerve compression site, providing more precise pain relief, which can often last for weeks to months.
👉 Note: ESI can control pain, but it cannot cure the underlying cause.
If you have bone spurs, sciatica, or a herniated disc, but don’t want to have surgery, what options do you have?
Before surgery, most patients may consider:
Rehabilitation therapy
Oral analgesics
Interventional pain management (such as epidural ESI injection)
These methods can temporarily relieve symptoms, improve quality of life, and buy time to monitor the condition.
How long does the effect of ESI last?
The pain relief usually begins to take effect 3–5 days after injection. The pain-relieving effect typically lasts for several weeks to several months. The duration of the effect depends on individual constitution, the severity of the cause, and the level of rehabilitation activity.
Is hospitalization required for ESI?
Most of these procedures are outpatient surgeries. Patients can return home after a 15-30 minute observation period following the procedure and do not require hospitalization.
How many times a year can I do ESI?
It is recommended to take steroids once every 3–4 months, and no more than 3–4 times a year, to avoid steroid side effects (such as osteoporosis, elevated blood sugar, and decreased immunity).
Can diabetic patients undergo ESI?
Yes, but the following is necessary:
Preoperative blood glucose assessment
Intensive blood glucose monitoring for 48–72 hours post-surgery, as steroids may temporarily raise blood glucose levels.
Can I have an ESI if I am taking anticoagulants or antiplatelet drugs?
Do not stop taking the medication on your own! You must:
have your doctor assess whether you need to stop taking the medication;
determine how long you need to stop and whether “bridging therapy” is necessary;
this is to ensure treatment safety and avoid the risk of bleeding or stroke.
After ESI, under what circumstances is it necessary to return for a follow-up appointment immediately?
Red flag symptoms requiring immediate return to the doctor or emergency room:
Fever, worsening redness, swelling, heat, and pain at the injection site
Progressive weakness or numbness in the lower extremities
Incontinence (urinary or fecal incontinence)
Severe headache (relieved by lying down, worsened by sitting up; may be a puncture headache)
Abnormal bleeding, large bruising
Severely uncontrolled blood sugar or blood pressure
**This website is intended to provide information on new medical developments and health education. Any discrepancies between the terms used in this content and those in the package insert (including descriptions of uses not covered by the approved indications or colloquial terms) are provided solely for the public’s understanding and reference; the official names of treatments and devices, as well as their effects, are subject to the physician’s personal explanation.
Related Articles
Regenerative Medicine Integrative Medicine Regenerative Therapy Please enter a title here Table of Contents Turning On the Body’s Repair Switch: How Does BMAC (Autologous High-Concentration Bone Marrow Concentrate) Reshape the Joint Microenvironment? Have you ever wondered why, even after multiple
Regenerative Medicine Integrative Medicine Regenerative Therapy Please enter a title here Table of Contents Unlocking the Joints’ Natural Healing Power: PRP Regenerative Therapy and a Holistic Anti-Aging Care Plan PRP (Platelet-Rich Plasma) is one of the core technologies in modern regenerative med
Regenerative Medicine Integrative Medicine Regenerative Therapy Please enter a title here Table of Contents All-Natural Tissue Regeneration | A Guide to the Sustained-Release Effects of PRF and Joint Self-Healing PRF (Platelet-Rich Fibrin) is a cutting-edge therapy in modern regenerative medicine. B
Regenerative Medicine Integrative Medicine instrument Please enter a title here Table of Contents MCS+ Blood Purification | Thorough Vascular Cleansing, Reducing the Risk of High Blood Pressure, High Cholesterol, and High Blood Sugar Why do modern people need blood purification? The high-pressure pa