Epidural Steroid Injection

Regen Health
2025-11-28
Spinal pain and leg numbness that just won't go away? A comprehensive analysis: 5 key indications and postoperative care for Epidural Injection.
Are you suffering from intermittent claudication that forces you to squat down and rest after walking only a short distance? Or do you experience deep, dull pain in your lower back when sitting for extended periods?
This article integrates the latest international journal evidence and common clinical treatment issues, comparing the three major procedures—TF, IL, and Caudal—to analyze the safety of ultrasound-guided injections, guiding you through the core value of this minimally invasive interventional therapy. Don’t let long-term nerve inflammation become permanent damage; learn now how to break the vicious cycle of “pain without movement” through precise injection.
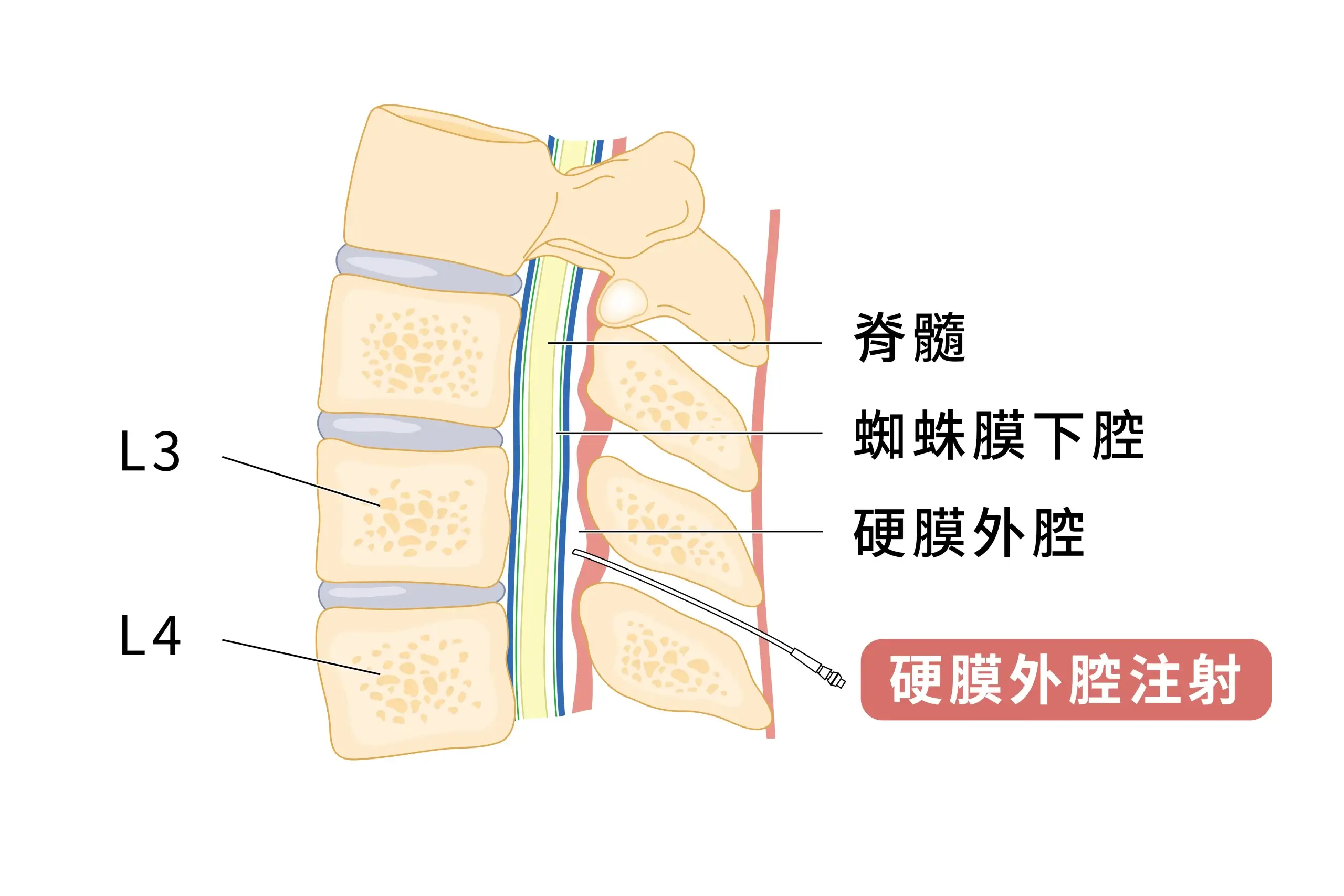
What is an Epidural Steroid Injection(ESI)?
The spinal nerves are encased in a protective membrane called the dura mater, and the space between this membrane and the vertebrae is the epidural space.
When a herniated disc or thickened ligamentum flavum compresses a nerve, the nerve root experiences severe mechanical compression and chemical inflammation.
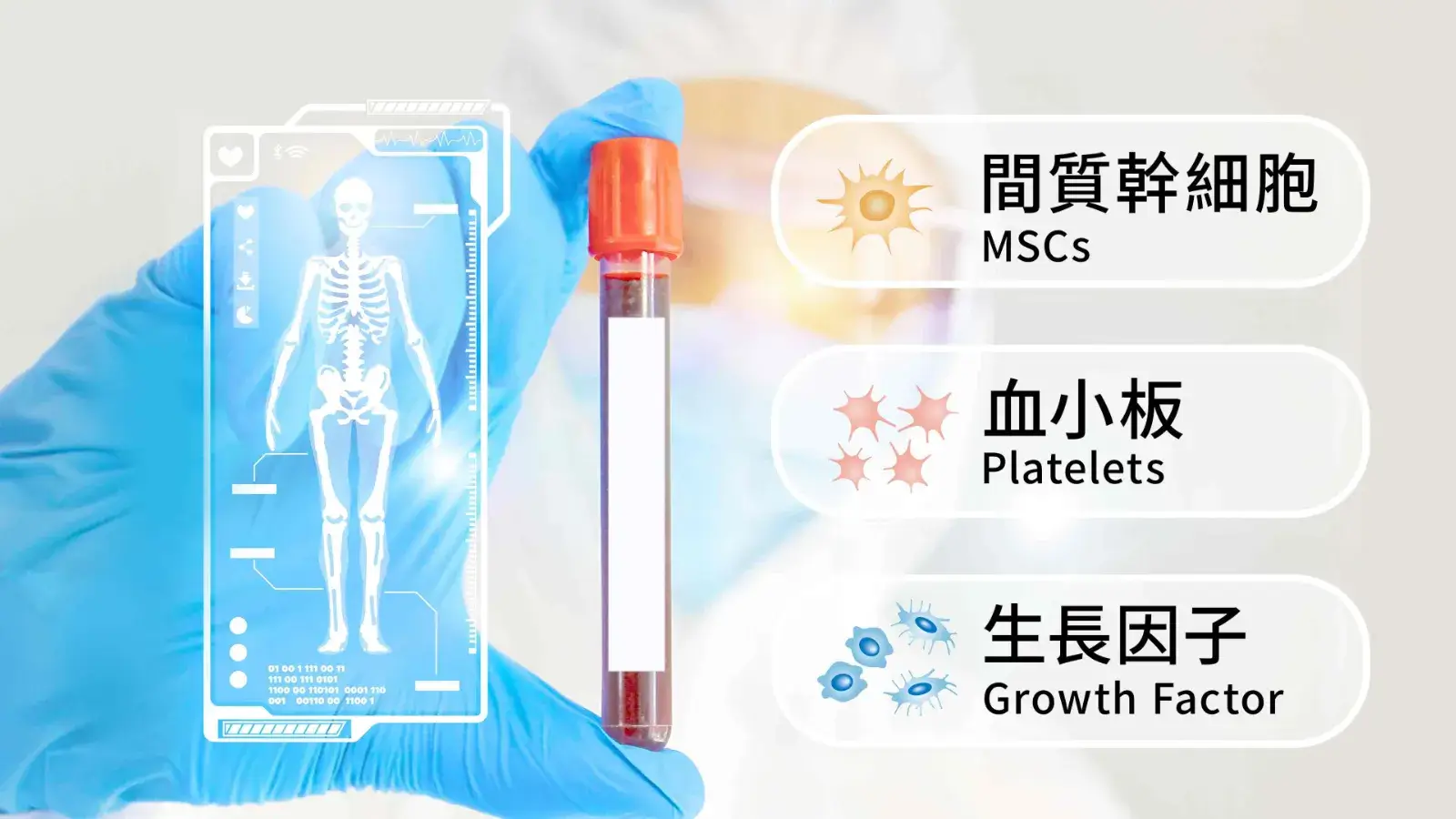
This procedure, guided by advanced imaging, precisely delivers high concentrations of anti-inflammatory drugs, anesthetics, or PRP (platelet-rich plasma) to this space, achieving:
Physical irrigation: Dilutes and removes pain-causing inflammatory factors around the nerve.
Chemical analgesia: Reduces nerve root edema and blocks pain signal transmission.
Biological repair: Provides growth factors (such as PRP) to promote the regeneration of damaged nerve tissue.
Three Injection Methods: Precise and Targeted Treatment
The physician will choose the appropriate injection site based on the individual’s MRI images and clinical symptoms:
|
Methods |
Indications |
Core Advantages |
|---|---|---|
|
Foraminal (TF) |
Herniated disc, unilateral sciatica |
Most precise! Medication can directly penetrate to the nerve’s exit point. |
| Interlaminar (IL) | Bilateral low back pain, multi-segmental degeneration |
Suitable for patients with severe structural deformities who are not suitable for lateral injection. |
|
Caudal |
Suitable for patients with severe structural deformities who are not suitable for lateral injection. |
High safety! Away from the spinal cord, suitable for frail or elderly individuals. |
Who is suitable for Epidural injection?
Epidural injection is a highly precise interventional treatment, particularly suitable for patients who are between those for whom conservative rehabilitation is ineffective and those for whom surgery is not yet necessary. This procedure can effectively relieve inflammation and improve quality of life if you have the following symptoms or diagnoses:
1. Disc Herniation/Spondylolisthesis – By injecting anti-inflammatory agents, it relieves nerve root edema caused by mechanical compression.
Symptoms: A herniated disc or displaced vertebra compresses a nerve root, causing radiating pain, numbness, or weakness in the buttocks and lower limbs, similar to an electric shock.
2. Sciatica – Administers medication precisely at the exit point of nerve compression, blocking pain signal transmission.
Symptoms: Typical pain pathway extends from the lower back to the buttocks, back of the thigh, and even down to the calf and foot.
3. Spinal Stenosis – Reduces inflammatory pressure within the constricted space, increasing walking distance and endurance.
Symptoms: The spinal canal narrows due to degeneration, compressing nerve bundles. Patients often experience “intermittent claudication” (leg and foot pain and numbness after walking a short distance, requiring rest to alleviate the symptoms).
4. Degenerative Disc Disease – Improves chemical inflammation caused by degeneration, relieving long-term dull pain.
Symptoms: Loss of disc height and decreased water content due to age or overuse leads to deep, chronic lower back pain, especially noticeable during prolonged sitting or posture changes.
5. Chronic Low Back Pain – Used as a diagnostic and treatment tool to help physicians identify the source of pain and break the vicious cycle of “pain without movement, and the less you move, the more pain you feel.”
Symptoms: Pain lasting more than three months and caused by a combination of factors (such as facet joint arthritis, chronic inflammation of muscles and ligaments).
Treatment Procedure and Postoperative Care
【Standard Treatment Procedure】
Imaging Confirmation: The physician reviews MRI or CT scans to determine the compressed segment.
Precise Needle Insertion: Local anesthesia is administered, and the needle is precisely inserted into the epidural space under image guidance. The procedure takes approximately 20 minutes.
Medication Administration: Anti-inflammatory drugs or regenerative agents (such as PRP) are selected based on the patient’s condition.
Postoperative Monitoring: Observe for 30 minutes. Patients can return home after confirming normal lower limb muscle strength.
【Precautions】 Golden Repair Period: Avoid strenuous heavy lifting for two weeks after injection. This period is crucial for nerve swelling reduction and repair.
Rehabilitation Cooperation: After pain relief, physical therapy should be initiated immediately to strengthen core muscles and prevent further deterioration of structural compression (such as slippage).
Epidural Steroid Injection(ESI) FAQ
Q1: Will epidural injections have long-term side effects like surgery?
No. This is an invasive, minimally invasive treatment, not surgery. The medication dosage is precisely calculated by a doctor, and most side effects are temporary muscle soreness or blood sugar fluctuations.
Q2: If I have bone spurs, can the injections eliminate them?
No. The injections are to address inflammation and pain caused by pressure. Structural problems like bone spurs require subsequent postural correction and core training for stabilization, or surgery may be considered in severe cases.
Q3: How long do the effects of epidural injections last?
According to 2024 literature, the average effect of a single injection lasts 3 to 6 months. The effect may be even longer if combined with PRP (post-inflammatory hyperplasia) repair therapy.
Q4: I’ve heard that steroid injections can cause osteoporosis?
Epidural injections use “local micro-dose steroids” and the frequency is limited (it is recommended not to exceed 3-4 times a year). Unlike the systemic side effects caused by long-term oral steroids, the public does not need to panic excessively.
Q5: When is epidural injection not suitable for me?
It is not recommended for those with injection site infection, abnormal coagulation function, or severe allergy to local anesthetics.
Q6: How many injections are needed for this treatment to be effective?
Is it a one-time treatment? It depends on the condition. > If it is inflammation caused by acute disc herniation, usually 1 to 2 injections will provide significant relief. However, if it is long-term spinal degeneration or stenosis, the doctor may plan a course of treatment (e.g., once every 2-4 weeks, for 3 consecutive times). The key point is: the injection is to “open the door to rehabilitation.” After the pain is reduced, core training is the key to preventing recurrence in the long term.
Q7: Can I go straight to work on the day of the injection? Or do I need to take a day off?
In principle, yes, but a “mini-vacation” is recommended. Although this is a minimally invasive procedure, there may be temporary soreness in the lower limbs for a few hours after the procedure. It is recommended to avoid high-pressure meetings or work that requires prolonged standing or lifting heavy objects on the day of treatment. Giving your body 24 hours to quietly absorb the medication before resuming normal work intensity the next day is a safer approach.
Q8: What symptoms require immediate follow-up after an epidural injection?
Although extremely rare, please contact your doctor immediately if you experience any of the following warning signs: Fever or abnormal redness, swelling, heat, and pain at the injection site: Infection risk needs to be ruled out. Severe headache: Especially headaches that hurt when sitting up and improve when lying down (this may be due to pressure changes caused by microleakage in the epidural space). Urinary or fecal incontinence or cauda equina syndrome: Sudden inability to urinate or numbness around the anus. Weakness in the lower limbs persisting for more than 24 hours without improvement.
Related Articles
Please enter a title here Regen Health Please enter a title here Is Your Shoulder Burning with Pain? Ultrasound-Guided Calcification Aspiration: Clinical Data from the Past Decade and a Comprehensive Treatment Guide Many patients are often awakened in the middle of the night or early morning by sev
Regen Health [The Complete Guide to Arthroscopic Cartilage Repair] Everything You Need to Know About the Minimally Invasive Procedure, Indications, and Postoperative Rehabilitation! Do you experience knee pain so severe that you can’t squat, feel your knee lock up after walking for a while, or even
Regen Health Say Goodbye to Joint Degeneration and Chronic Pain: A Guide to PRP Regenerative Therapy Injections, Cost Estimates, and Non-Surgical Treatment PRP (Platelet-Rich Plasma) therapy is a clinically proven, non-surgical regenerative medicine technique. By drawing approximately 10–15 cc of th
Regen Health Advanced PRP Therapy | The Golden Treatment for Activating the "Self-Repair" Mechanism of Joints and Tendons PRF is a highly safe, naturally derived regenerative medicine therapy that utilizes growth factors and fibrin structures from the patient’s own blood to help the body a
Regen Health No Hospital Stay Required! The Complete Guide to BMAC Autologous Bone Marrow Concentrate Injection Therapy When traditional regenerative therapies or hyaluronic acid fail to address severe joint degeneration, BMAC (Bone Marrow Aspirate Concentrate) offers a more advanced option. This i
Regen Health Minimally Invasive Release Surgery for "Mom's Hand" | Say Goodbye to Thumb and Wrist Pain and Regain Full Mobility What Is "Mom's Hand"? (Definition of De Quervain's Syndrome) The medical term for "mom's hand" is stenosing tenosynovitis