Pain and Anesthesia
Various Anesthesia
Pain and Anesthesia
Various Anesthesia
Various Anesthesia
Various Anesthesia
Nerve Block Injection
Chronic Pain Management
General Anesthesia
Table of Contents
Understanding General Anesthesia: Ensuring Safety During Major Surgeries—A Comprehensive Guide to the Process, Risks, and Differences in Intubation
During major or medium-sized surgeries or lengthy medical procedures, “general anesthesia” is a core technique that ensures the smooth progression of the surgery and safeguards the patient’s safety and comfort. Many patients feel anxious about “intubation” or “losing consciousness.” This article will provide an in-depth look at how general anesthesia works, the two main methods of respiratory management, and the safety protocols that must be followed before surgery.
What is general anesthesia?
General anesthesia is currently the most comprehensive and deepest form of anesthesia. Through intravenous administration of medications, it induces a state of deep sleep in which the patient experiences no pain and complete muscle relaxation. Throughout the procedure, the anesthesiologist controls the patient’s breathing and continuously monitors vital signs such as heart rate, blood pressure, and blood oxygen levels. Indications
and types of surgery:
- Major surgeries: Such as major procedures involving the chest or abdomen.
- Long-duration surgeries: Procedures expected to last more than 2 hours.
- Specific surgical sites: Procedures that cannot be performed under regional anesthesia.
- Special requirements: Procedures requiring complete muscle relaxation.
Airway Management: What Is the Difference Between an LMA and Endotracheal Intubation?
During general anesthesia, patients lose the ability to breathe on their own, so the physician will select the appropriate respiratory management device based on the surgical requirements:
1. Laryngeal Mask Airway (LMA) | Gentle and non-invasive
- Procedure: A flexible mask is placed in the lower pharynx to cover the opening of the trachea without entering the trachea.
- Advantages: Minimal throat irritation; postoperative coughing, sore throat, or hoarseness are less common.
- Suitable for: Most short-duration outpatient surgeries involving moderate pain.
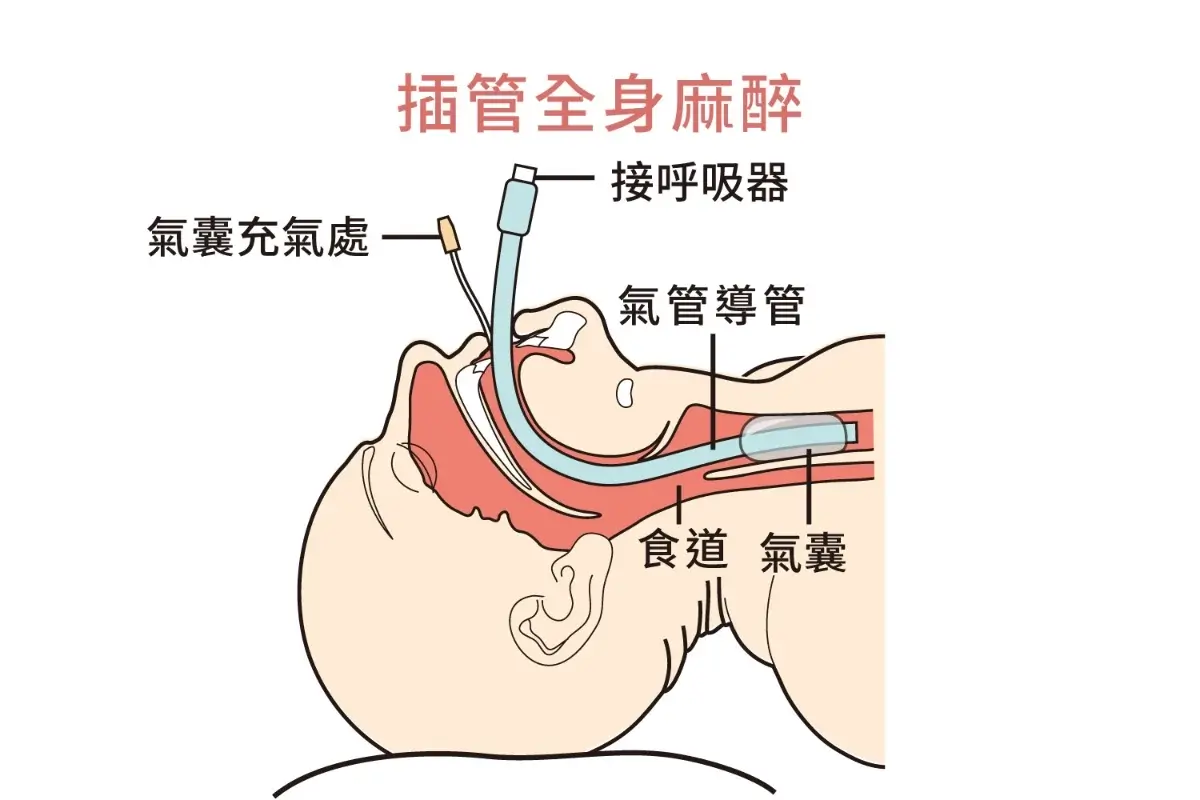
2. Intubated General Anesthesia (Intubated GA) | Highest Safety and Stability
- Procedure: An endotracheal tube is inserted into the trachea, and breathing is precisely controlled by a machine.
- Advantages: Provides the highest level of respiratory stability and can handle complex situations during high-risk or major surgeries.
- Indications: Long-duration surgeries or procedures requiring complete control of muscle tone.
Risks of General Anesthesia and Postoperative Side Effects
Modern anesthesia techniques are highly advanced, but they may still cause some temporary discomfort:
- Common symptoms: sore throat, sensation of a foreign body in the throat, cough (usually improves within 2–5 days), dizziness, nausea, vomiting, weakness, and chills.
- Rare risks: heart attack, stroke, anaphylactic shock (more common in patients with underlying chronic conditions).
- Special circumstances: Tooth loss (higher risk for those with pre-existing loose teeth) or airway edema.
Preoperative Safety Preparations for General Anesthesia: Fasting and Communication Regarding Medication
Adhering to preoperative guidelines is key to reducing anesthesia risks:
1. Strict fasting guidelines:
- Fatty foods: Fast for 8 hours.
- Light meals (such as white toast, hard-boiled eggs): Fast for 6 hours.
- Water: Do not drink for 2 hours.
Note: Fasting is required to prevent aspiration pneumonia caused by vomiting.
2. Guidelines for Discontinuing GLP-1 (weight-loss injections):
- Weekly formulation (injected weekly): Discontinue use 7 days prior to surgery.
- Daily formulation (daily injection): Discontinue use 24 hours prior to surgery.
Note: These medications delay gastric emptying and increase anesthesia risks.
3. Full disclosure of medical history: This includes chronic conditions (heart, lung, and kidney diseases; hypertension, hyperlipidemia, and diabetes), respiratory abnormalities (such as obstructive sleep apnea [OSA]), coagulation disorders, and allergy history.
Frequently Asked Questions About General Anesthesia
Is it normal to have a sore throat after waking up from general anesthesia with intubation?
Normal. This is due to mild irritation of the endotracheal tube to the mucous membrane, which usually improves within 1–3 days. Drinking plenty of water can help relieve the symptoms.
Can I have general anesthesia if I have a chronic illness?
Yes, it’s possible. However, chronic illnesses increase the risks. The anesthesiologist will design the safest plan based on your health condition, so please be sure to disclose this information honestly before the procedure.
How long does it take to wake up after general anesthesia?
After the surgery is completed and the anesthesia is discontinued, the doctor will remove the breathing tube, and the patient will immediately wake up and be transferred to the recovery room for observation.
Why should gel nails be removed and makeup prohibited before the procedure?
This is so that doctors can accurately monitor your blood oxygenation status through nail color and pulse oximeter, ensuring safety during the procedure.
What is the difference between general anesthesia and intravenous anesthesia?
Intravenous anesthesia is considered “mild to moderate” general anesthesia, allowing the patient to breathe independently; general anesthesia is deeper and usually requires machine-assisted breathing, making it suitable for more complex surgeries.
Will the Laryngeal Mask (LMA) fall off?
The LMA is placed by a professional anesthesiologist, and vital signs are continuously monitored during the procedure. It is highly safe and gentler than intubation.
What if I wake up during surgery?
An anesthesiologist will monitor the depth of anesthesia throughout the procedure, maintaining deep sleep and a pain-free state, and cases of patients waking up during surgery are extremely rare.
What situations require a follow-up appointment after surgery?
If you experience difficulty breathing, persistent chest pain, confusion, or a persistent high fever, contact medical personnel immediately.
**This website is intended to provide information on new medical developments and health education. Any discrepancies between the terms used in this content and those in the package insert (including descriptions of uses not covered by the approved indications or colloquial terms) are provided solely for the public’s understanding and reference; the official names of treatments and devices, as well as their effects, are subject to the physician’s personal explanation.
Related Articles
Regenerative Medicine Integrative Medicine Regenerative Therapy Please enter a title here Table of Contents Turning On the Body’s Repair Switch: How Does BMAC (Autologous High-Concentration Bone Marrow Concentrate) Reshape the Joint Microenvironment? Have you ever wondered why, even after multiple
Regenerative Medicine Integrative Medicine Regenerative Therapy Please enter a title here Table of Contents Unlocking the Joints’ Natural Healing Power: PRP Regenerative Therapy and a Holistic Anti-Aging Care Plan PRP (Platelet-Rich Plasma) is one of the core technologies in modern regenerative med
Regenerative Medicine Integrative Medicine Regenerative Therapy Please enter a title here Table of Contents All-Natural Tissue Regeneration | A Guide to the Sustained-Release Effects of PRF and Joint Self-Healing PRF (Platelet-Rich Fibrin) is a cutting-edge therapy in modern regenerative medicine. B
Regenerative Medicine Integrative Medicine instrument Please enter a title here Table of Contents MCS+ Blood Purification | Thorough Vascular Cleansing, Reducing the Risk of High Blood Pressure, High Cholesterol, and High Blood Sugar Why do modern people need blood purification? The high-pressure pa