Is PRP/PRF Really Effective for Degenerative Knee Osteoarthritis? Doctor Explains 6 Major Regenerative Repair Mechanisms

Xu Fang-Wei (Orthopedic Physician, Regen Clinic), Medical License No. 002188
2026-01-12

For degenerative knee osteoarthritis, conventional treatments can only relieve pain, whereas PRP (platelet-rich plasma) and PRF (platelet-rich fibrin) work through six scientifically proven mechanisms—“promoting cartilage regeneration,” “modulating inflammation,” and “improving mitochondrial function,” among others—to slow degeneration at its source. This article is an in-depth analysis by Dr. Hsu Fang-Wei of Regen Clinic, Songshan District, explaining the regenerative medicine principles and clinical indications of platelet therapies.
Why Are More Knee Degeneration Patients Choosing PRP/PRF?
In my orthopedic clinic in Songshan District, degenerative knee osteoarthritis (Knee Osteoarthritis) is the most common condition and the one that troubles many elderly patients the most. After examinations at major hospitals, the standard protocol is often: “take anti-inflammatory medication, undergo physical therapy, try hyaluronic acid injections if ineffective, and ultimately consider joint replacement.”
However, for many patients who still wish to maintain their quality of life, pain, limping while walking, and discomfort when turning at night make it impossible to wait passively. Therefore, in recent years, platelet-based regenerative therapies such as PRP (Platelet-Rich Plasma) and PRF (Platelet-Rich Fibrin) have become popular options that patients actively inquire about.
As a physician, I must return to the scientific evidence to answer the most crucial question: “Do PRP/PRF really work for degenerative knee osteoarthritis?”
Evidence-Based Insights: How Platelet Preparations Repair Degenerated Knees
To determine whether it is “effective,” we cannot rely solely on subjective feeling; understanding the mechanisms of regenerative medicine is essential. PRP and PRF are not merely pain relievers—they are rich in growth factors and can influence joint inflammation, cartilage metabolism, and cell survival through multiple biological mechanisms.
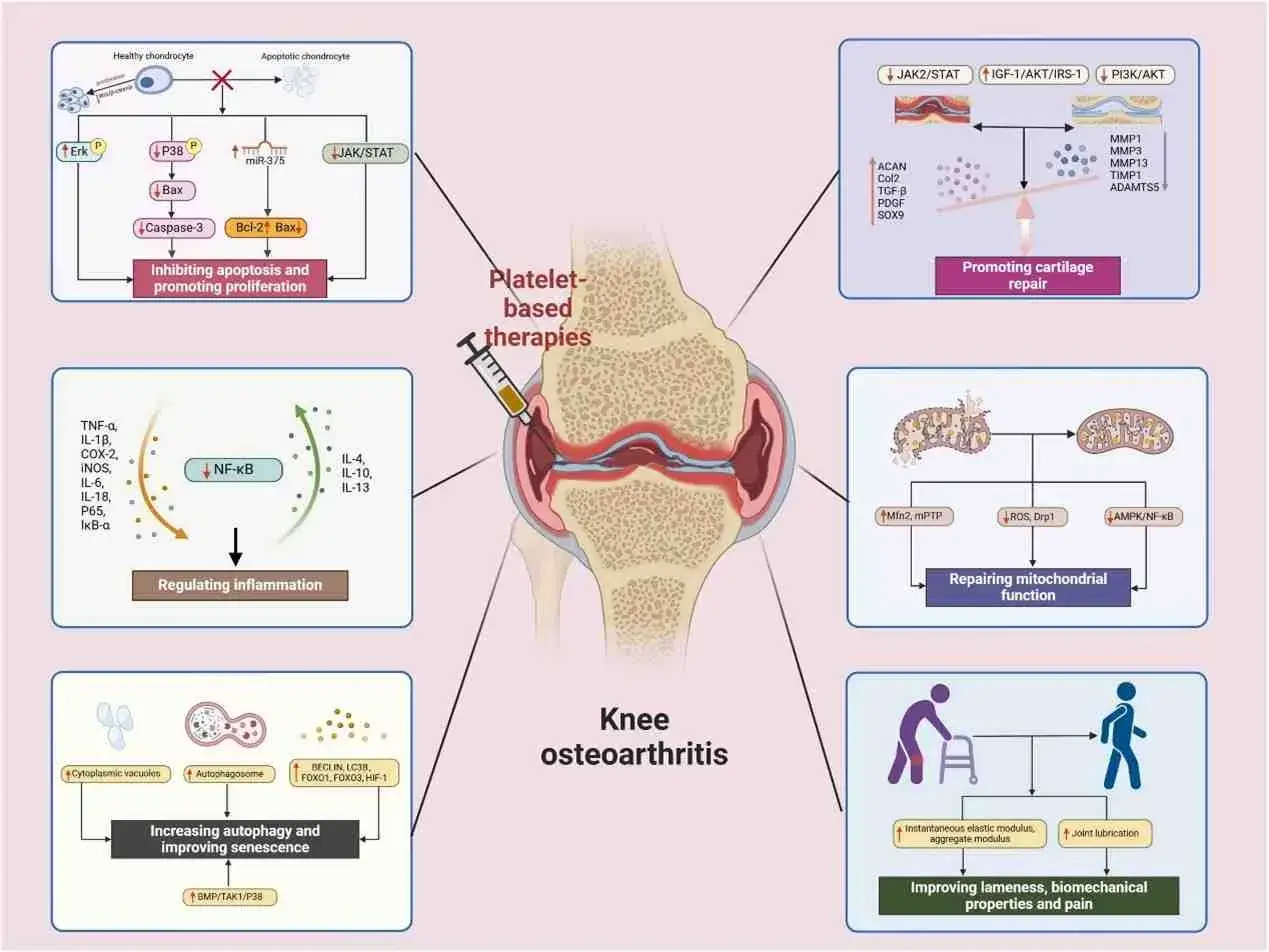
According to the latest biomedical literature in 2024, we have summarized 6 clinically proven regenerative mechanisms:
1. Promote chondrocyte proliferation and inhibit apoptosis (Anti-Apoptosis)
PRP helps maintain normal chondrocyte morphology. Studies show that, with dose adjustment, PRP can regulate miRNA and cell cycle pathways to effectively reduce chondrocyte apoptosis (cell death), thereby activating the tissue’s self-repair capability. (Reference: Exp. Cell Res, 2017)
2. Improve cartilage matrix metabolism and reconstruct structure
The core issue of degeneration is that cartilage becomes “soft and brittle.” Platelet therapies can increase the density of the cartilage matrix and regulate repair signals, reducing inflammation in the subchondral bone, thereby assisting cartilage repair structurally.
3. Block inflammatory factors and relieve chronic pain
Knee pain is not solely caused by wear—it is largely due to “inflammation.” Multiple studies indicate that PRP/PRF can inhibit inflammatory signaling pathways, reduce the release of inflammatory factors, and prevent continuous degradation of the cartilage matrix by inflammatory substances. (Reference: Immunopharmacol. Immunotoxicol., 2022)
4. Repair mitochondrial function and provide antioxidant effects (Mitochondrial Repair)
This is a recent discovery in functional medicine. Chondrocyte apoptosis is related to “mitochondrial dysfunction.” Platelet therapies can reduce damage caused by reactive oxygen species (ROS) and, through AMPK/NF-κB signaling regulation, protect chondrocytes from oxidative stress. (Reference: Tissue Cell, 2022)
5. Activate autophagy to delay aging (Autophagy)
Autophagy is a crucial cellular mechanism for removing internal waste and combating aging. Research confirms that platelet therapies can induce autophagy in chondrocytes, reverse the cellular aging process, and enhance cell survival.
6. Improve biomechanics: walk more steadily and with less pain
This is the change most noticeable to patients. Animal experiments and clinical data show that after treatment:
- Cartilage thickness increases
- Joint lubrication improves
- Improvement in limping and pain scores
Orthopedic Physician Summary: The Role of PRP/PRF in Treatment
Based on current evidence-based medicine, we can summarize four major functions of platelet therapies in the treatment of degenerative arthritis:
- Modulate intra-articular inflammation (Anti-inflammation)
- Improve cartilage matrix structure (Matrix Restoration)
- Inhibit chondrocyte apoptosis (Cell Survival)
- Promote repair and survival (Regeneration)
In short, for patients who want to avoid surgery or for whom painkillers are ineffective, the value of PRP/PRF lies in: “reducing inflammatory pain, slowing degeneration, and improving mobility.”
Key Concept: PRP Results Vary from Person to Person
This is a concept that Dr. Hsu Fang-Wei particularly emphasizes in his clinic. Although the mechanisms have scientific support, clinical outcomes can be influenced by the following individual factors:
- Severity of knee osteoarthritis (patients with stage IV severe wear may have limited effect)
- Body weight and load-bearing habits (excess weight can offset the repair effect)
- Exercise and lifestyle
- Work posture
Therefore, PRP or PRF is not a cure-all. Whether it is suitable for injection must be evaluated by a professional orthopedic physician using X-ray or ultrasound to create a personalized treatment plan, rather than relying solely on online cases.
When to See an Orthopedic Physician for Knee Pain
If you live in Taipei’s Songshan District or nearby and experience any of the following symptoms, it is recommended to undergo a comprehensive evaluation as soon as possible:
- ❌ Deep knee pain when walking
- ❌ Pain that wakes you at night when turning in bed
- ❌ Weakness or difficulty going up and down stairs
- ❌ Already diagnosed with degenerative knee osteoarthritis
Regenerative medicine treatments (PRP/PRF) are recommended to be combined with lifestyle adjustments and physical therapy to achieve the best long-term pain relief outcomes.
PRP Platelet Clinical Research International Journal References
To ensure the scientific accuracy of the information, this article cites the following international journal studies:
- Mechanisms and applications of the regenerative capacity of platelets-based therapy in knee osteoarthritis. Biomedicine & Pharmacotherapy 178 (2024) 117226
- Platelet rich plasma (PRP) induces chondroprotection… Exp. Cell Res, 352 (1) (2017)
- Platelet-rich plasma treatment alleviates osteoarthritis-related pain… Immunopharmacol. Immunotoxicol., 44 (1) (2022)
- Recombinant platelet-derived growth factor-BB alleviates osteoarthritis… J. Cell. Mol. Med., 25 (15) (2021)
- Platelet-rich plasma contributes to chondroprotection by repairing mitochondrial function… Tissue Cell, 77 (2022) (and other studies on autophagy and arthritis)
[Disclaimer] This article was compiled by Dr. Hsu Fang-Wei based on evidence-based medical literature and is intended to provide medical education information. Actual treatment methods, dosages, and outcomes may vary for each individual. Please visit a medical facility in person for a professional evaluation and diagnosis tailored to your specific condition.
Related Articles
Please enter a title here Hsu Fang-wei (Orthopedic Surgeon at Jianli Clinic) | Orthopedic Specialist License No. 002188 Please enter a title here What Is Piriformis Syndrome? A Common Nerve Compression Problem in People Who Sit for Long Periods Every time you walk into an office or a coffee shop, t
Please enter a title here Hsu Fang-wei (Orthopedic Surgeon at Jianli Clinic) | Orthopedic Specialist License No. 002188 Please enter a title here Lately, in my clinic, I often see middle-aged women rush in, looking panicked, pointing to the middle joint of their finger and asking, “Doctor, is my fin
Regen Health Don’t Let the “Three Lows” Steal Your Quality of Life in Old Age We often hear about the dangers of the “Three Highs” (high blood pressure, high cholesterol, high blood sugar). However, as Taiwan officially enters a super-aged society in 2025, few pay attention to the equally critical